Chinese Medical Sciences Journal ›› 2020, Vol. 35 ›› Issue (3): 262-271.doi: 10.24920/003668
术前中性粒细胞与淋巴细胞比值预测可切除泌尿系肿瘤预后的价值:系统综述和荟萃分析
- 中国医学科学院 北京协和医院医学院,北京协和医学院泌尿外科,北京 100730
-
收稿日期:2020-01-08出版日期:2020-09-30发布日期:2020-09-25 -
通讯作者:张玉石 E-mail:beijingzhangyushi@126.com
Value of Preoperative Neutrophil-to-Lymphocyte Ratio in Predicting Prognosis of Surgically Resectable Urinary Cancers: Systematic Review and Meta-Analysis
Wang Zhan,Wang Xu,Wang Wenda,Zheng Guoyang,Guo Hao,Zhang Yushi( )
)
- Department of Urology, Peking Union Medical College Hospital, Chinese Academy of Medical Sciences & Peking Union Medical College, Beijing 100730, China
-
Received:2020-01-08Published:2020-09-30Online:2020-09-25 -
Contact:Zhang Yushi E-mail:beijingzhangyushi@126.com
摘要:
目的 术前中性粒细胞与淋巴细胞比值(NLR)与多种恶性肿瘤的预后密切相关,但是,NLR对可切除泌尿系肿瘤预后的影响尚不确定。因此,此系统综述和荟萃分析旨在探讨术前NLR在预测可切除泌尿系肿瘤预后方面的价值。
方法 我们通过检索Embase、PubMed/MEDLINE和Cochrane数据库,依据纳入和排除标准筛选文献,最终纳入25项研究,其中包括15950例受试对象。采用风险比(HRs)及其95%可信区间(CIs)评估术前NLR与可切除泌尿系肿瘤患者的总生存期(OS)及肿瘤特异性生存期(CSS)的关系。
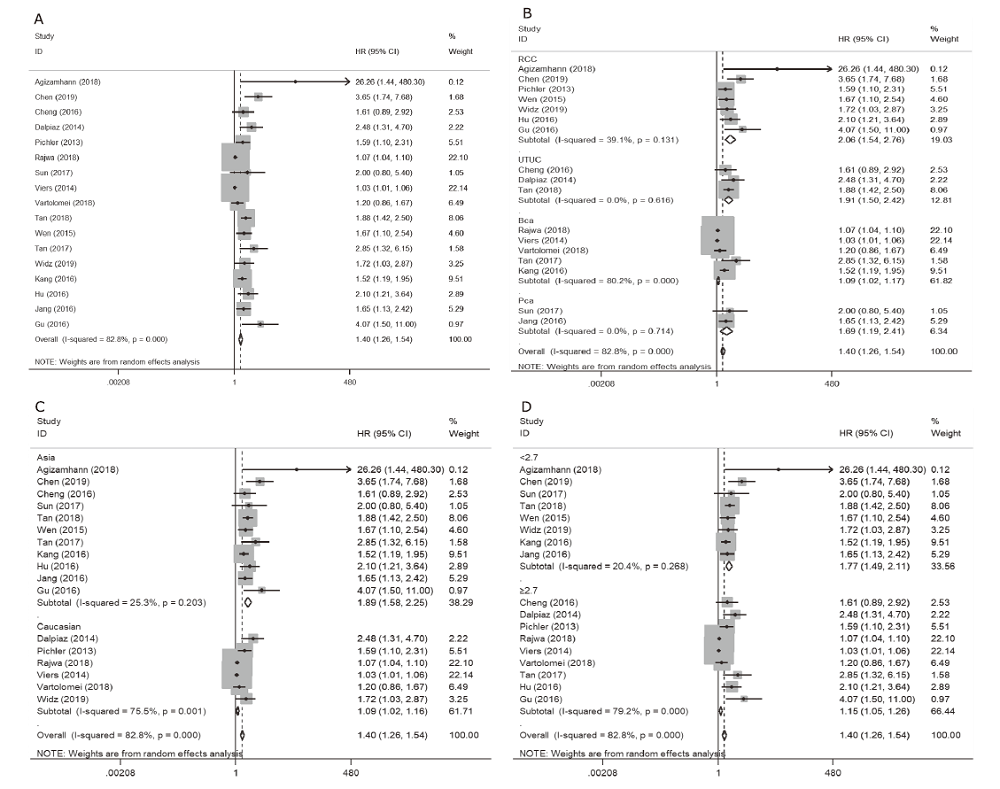
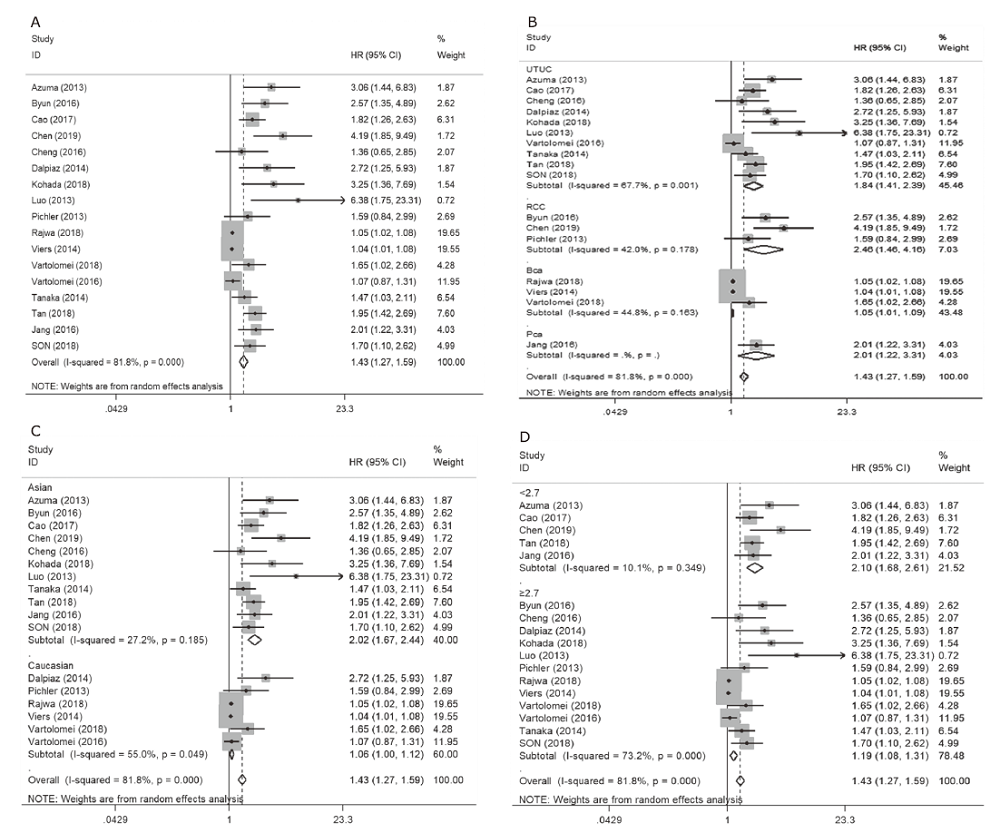
结果 结果表明对于患有可切除泌尿系恶性肿瘤的患者,术前NLR能预测其预后。NLR越高,患者的OS(HR=1.40,95%CI:1.26~1.54,P<0.001)和CSS越短(HR=1.43,95%CI:1.27~1.59,P<0.001)。此外,不论患者种族或术前NLR阈值高低,术前NLR升高均能提示肾细胞癌(OS:HR=2.06,95%CI=1.54~2.76,P=0.131;CSS:HR=2.46,95%CI=1.46~4.16,P=0.178)、上尿路上皮癌(OS:HR=1.91,95%CI=1.50~2.42,P=0.616;CSS:HR=1.84,95%CI=1.41~2.39,P=0.001)、膀胱癌(OS:HR=1.09,95%CI=1.02~1.17,P<0.001;CSS:HR=1.05,95%CI=1.01~1.09,P=0.163)和前列腺癌(OS:HR=1.69,95%CI=1.19~2.41,P=0.714)预后较差。
结论 术前NLR升高能够作为预测泌尿系可切除恶性肿瘤不良预后的指标,包括肾癌、膀胱癌、前列腺癌和上尿路上皮癌。
引用本文
Wang Zhan, Wang Xu, Wang Wenda, Zheng Guoyang, Guo Hao, Zhang Yushi. Value of Preoperative Neutrophil-to-Lymphocyte Ratio in Predicting Prognosis of Surgically Resectable Urinary Cancers: Systematic Review and Meta-Analysis[J].Chinese Medical Sciences Journal, 2020, 35(3): 262-271.
"
| Author | Year | Country | Tumor type | No. of Patients | Age (yrs) | Gender (M:F) | Cut-off value | Follow-up (months) | Outcomes | Analysis type |
|---|---|---|---|---|---|---|---|---|---|---|
| Son et al.[ | 2018 | Korea | UTUC | 1137 | 69 (61-74)* | 825:312 | 3.3 | 39.1 (18.3-63.8)* | RFS, CSS | UV, MV |
| Azuma et al.[ | 2013 | Japan | UTUC | 137 | 69.4 (40-88) | 106:31 | 2.5 | 60.9 (1.9-187.3) | RFS, CSS | UV, MV |
| Kohada et al.[ | 2018 | Japan | UTUC | 148 | 71 (64-78)* | 112:36 | 3 | 35.5 (12-66)* | RFS, CSS | UV, MV |
| Tanaka et al.[ | 2014 | Japan | UTUC | 665 | 70 (62-76)* | 493:172 | 3 | 28 (14-57)* | RFS, CSS | UV, MV |
| Cao et al.[ | 2017 | China | UTUC | 656 | 68 (39-88) | 290:366 | 2.4 | 46 (12-144) | IVRFS, CSS | UV, MV |
| Cheng et al.[ | 2016 | China | UTUC | 195 | 68±10.3 | 79:116 | 2.7 | 36 | OS, CSS | UV, MV |
| Luo et al.[ | 2014 | China | UTUC | 234 | N | 102:132 | 3 | 40.7±23.8 | MFS, CSS | UV, MV |
| Tan et al.[ | 2018 | China | UTUC | 717 | 67 (59-74)* | 408:309 | 2.5 | 42 (18-76)* | OS, DFS, CSS, MFS | MV |
| Dalpiaz et al.[ | 2014 | Austria | UTUC | 202 | 69.3 (32-85) | 122:80 | 2.7 | 45 (0-199) | CSS, OS | UV, MV |
| Vartolomei et al.[ | 2017 | Austria | UTUC | 2274 | 69 (61-76) | 1527:747 | 2.7 | 40 (20-76) | RFS, CSS | UV, MV |
| Byun et al.[ | 2016 | Korea | RCC | 1284 | 55.9±12.9 | 913:371 | 3.7 | 39 (19-69)* | RFS, CSS | MV |
| Widz et al.[ | 2020 | Poland | RCC | 196 | 61 (24-85)* | 116:80 | 2.69 | 68 (44.5-78) | OS | UV, MV |
| Agizamhann et al.[ | 2018 | China | RCC | 82 | 37 (2-71) | 33:49 | 2.45 | 31 (2-108) | OS, DFS | UV, MV |
| Chen et al.[ | 2019 | China | RCC | 414 | 56.3 (24-80) | 257:157 | 2.17 | 69.2 (1-151) | OS, CSS | MV |
| Wen et al.[ | 2015 | China | RCC | 327 | 56 (3-86) | 211:116 | 1.7 | 43 (0-97) | OS, DFS | UV, MV |
| Hu et al.[ | 2017 | China | RCC | 484 | 56 (21-81) | 278:206 | 2.78 | 36 | OS | UV, MV |
| Gu et al.[ | 2016 | China | RCC | 103 | 56 (16-79) | 71:32 | 4.1 | 19.9 (10.8-35.1)* | OS | UV, MV |
| Pichler et al.[ | 2013 | Austria | RCC | 678 | N | N | 3.3 | 44 (0-130) | OS, CSS | UV, MV |
| Jang et al.[ | 2016 | Korea | Pca | 2067 | 66 (61-70) | N | 1.76 | 78 (65-6)* | BCRFS, CSS, OS | UV, MV |
| Sun et al.[ | 2018 | China | Pca | 226 | N | N | 2.31 | 24 (1-73) | OS, DFS | UV, MV |
| Viers et al.[ | 2014 | USA | Bca | 899 | 69 (62-76)* | 723:176 | 2.7 | 130.8 (99.6-166.8)* | DFS, CSS, OS | UV, MV |
| Tan et al.[ | 2017 | Singapore | Bca | 84 | 67 (37-82) | 63:21 | 2.7 | 30.1 (3.2-161.7) | DFS, OS | UV, MV |
| Kang et al.[ | 2017 | Korea | Bca | 1551 | 65 (57-72)* | 1302:249 | 2 | 52 (27-82)* | OS | UV, MV |
| Rajwa et al.[ | 2018 | Poland | Bca | 144 | N | N | 3 | 14 (7-40)* | OS, CSS | UV, MV |
| Vartolomei et al.[ | 2018 | Italy | Bca | 1046 | 70 (29-91) | 864:182 | 3 | 26 (10-47)* | OS, DFS, CSS | MV |
"
| Subgroups | No. of studies | No. of patients | HR | 95%CI | Pheterogeneity |
|---|---|---|---|---|---|
| Tumor type | |||||
| RCC | 7 | 2284 | 2.06 | 1.54-2.76 | 0.131 |
| UTUC | 3 | 1114 | 1.91 | 1.50-2.42 | 0.616 |
| Bca | 5 | 3724 | 1.09 | 1.02-1.17 | <0.001 |
| Pca | 2 | 2293 | 1.69 | 1.19-2.41 | 0.714 |
| Ethnicity | |||||
| Asian | 11 | 3165 | 1.89 | 1.58-2.25 | 0.203 |
| Caucasian | 6 | 6250 | 1.09 | 1.02-1.16 | 0.001 |
| Cut-off value | |||||
| < 2.7 | 8 | 5580 | 1.77 | 1.49-2.11 | 0.268 |
| ≥2.7 | 9 | 3835 | 1.15 | 1.05-1.26 | <0.001 |
| Overall | 17 | 9415 | 1.40 | 1.26-1.54 | <0.001 |
"
| Subgroups | No. of studies | No. of patients | HR | 95%CI | Pheterogeneity |
|---|---|---|---|---|---|
| Tumor type | |||||
| RCC | 3 | 2376 | 2.46 | 1.46-4.16 | 0.178 |
| UTUC | 10 | 6365 | 1.84 | 1.41-2.39 | 0.001 |
| Bca | 3 | 2089 | 1.05 | 1.01-1.09 | 0.163 |
| Pca | 1 | 2067 | * | * | * |
| Ethnicity | |||||
| Asian | 11 | 7654 | 2.02 | 1.67-2.44 | 0.185 |
| Caucasian | 6 | 5243 | 1.06 | 1.00-1.12 | 0.049 |
| Cut-off value | |||||
| < 2.7 | 5 | 3991 | 2.10 | 1.68-2.61 | 0.349 |
| ≥2.7 | 12 | 8906 | 1.19 | 1.08-1.31 | <0.001 |
| Overall | 17 | 12897 | 1.43 | 1.27-1.59 | <0.001 |
| 1. |
Siegel RL, Miller KD, Jemal A. Cancer statistics, 2019. CA Cancer J Clin 2019; 69(1):7-34. doi: 10.3322/caac.21551.
doi: 10.3322/caac.21551 pmid: 30620402 |
| 2. |
Widz D, Mitura P, Buraczynski P, et al. Preoperative neutrophil-lymphocyte ratio as a predictor of overall survival in patients with localized renal cell carcinoma. Urol J 2020; 17(1):30-5. doi: 10.22037/uj.v0i0.4541.
doi: 10.22037/uj.v0i0.4541 pmid: 31087321 |
| 3. |
Jang WS, Cho KS, Kim KH, et al. Prognostic impact of preoperative neutrophil-to-lymphocyte ratio after radical prostatectomy in localized prostate cancer. Prostate Cancer Prostatic Dis 2016; 19(3):298-304. doi: 10.1038/pcan.2016.20.
doi: 10.1038/pcan.2016.20 pmid: 27349499 |
| 4. |
Kang M, Jeong CW, Kwak C, et al. Preoperative neutrophil-lymphocyte ratio can significantly predict mortality outcomes in patients with non-muscle invasive bladder cancer undergoing transurethral resection of bladder tumor. Oncotarget 2017; 8(8):12891-901. doi: 10.18632/oncotarget.14179.
pmid: 28039452 |
| 5. |
Chen Z, Wang K, Lu H, et al. Systemic inflammation response index predicts prognosis in patients with clear cell renal cell carcinoma: a propensity score-matched analysis. Cancer Manag Res 2019; 11:909-19. doi: 10.2147/CMAR.S186976.
pmid: 30697081 |
| 6. |
Vartolomei MD, Ferro M, Cantiello F, et al. Validation of neutrophil-to-lymphocyte ratio in a multi-institutional cohort of patients with T1G3 non-muscle-invasive bladder cancer. Clin Genitourin Cancer 2018; 16(6):445-52. doi: 10.1016/j.clgc.2018.07.003.
doi: 10.1016/j.clgc.2018.07.003 pmid: 30077463 |
| 7. |
Tan P, Xu H, Liu L, et al. The prognostic value of preoperative neutrophil-to-lymphocyte ratio in patients with upper tract urothelial carcinoma. Clin Chim Acta 2018; 485:26-32. doi: 10.1016/j.cca.2018.06.019.
pmid: 29908941 |
| 8. |
Sun Z, Ju Y, Han F, et al. Clinical implications of pretreatment inflammatory biomarkers as independent prognostic indicators in prostate cancer. J Clin Lab Anal 2018; 32(3):e22277. doi: 10.1002/jcla.22277.
doi: 10.1002/jcla.2018.32.issue-3 |
| 9. |
Son S, Hwang EC, Jung SI, et al. Prognostic value of preoperative systemic inflammation markers in localized upper tract urothelial cell carcinoma: a large, multicenter cohort analysis. Minerva Urol Nefrol 2018; 70(3):300-9. doi: 10.23736/s0393-2249.18.02914-4.
doi: 10.23736/S0393-2249.18.02914-4 pmid: 29381018 |
| 10. |
Rajwa P, ?yczkowski M, Paradysz A, et al. Evaluation of the prognostic value of LMR, PLR, NLR, and dNLR in urothelial bladder cancer patients treated with radical cystectomy. Eur Rev Med Pharmacol Sci 2018; 22(10):3027-37. doi: 10.26355/eurrev_201805_15060.
doi: 10.26355/eurrev_201805_15060 pmid: 29863247 |
| 11. |
Kohada Y, Hayashi T, Goto K, et al. Preoperative risk classification using neutrophil-lymphocyte ratio and hydronephrosis for upper tract urothelial carcinoma. Jpn J Clin Oncol 2018; 48(9):841-50. doi: 10.1093/jjco/hyy084.
pmid: 30085174 |
| 12. |
Agizamhan S, Qu F, Liu N, et al. Preoperative neutrophil-to-lymphocyte ratio predicts the surgical outcome of Xp11.2 translocation/TFE3 renal cell carcinoma patients. BMC Urol 2018; 18(1):60. doi: 10.1186/s12894-018-0374-z.
doi: 10.1186/s12894-018-0374-z pmid: 29890986 |
| 13. |
Vartolomei MD, Mathieu R, Margulis V, et al. Promising role of preoperative neutrophil-to-lymphocyte ratio in patients treated with radical nephroureterectomy. World J Urol 2017; 35(1):121-30. doi: 10.1007/s00345-016-1848-9.
doi: 10.1007/s00345-016-1848-9 pmid: 27209168 |
| 14. |
Tan YG, Eu E, Lau Kam On W, et al. Pretreatment neutrophil-to-lymphocyte ratio predicts worse survival outcomes and advanced tumor staging in patients undergoing radical cystectomy for bladder cancer. Asian J Urol 2017; 4(4):239-46. doi: 10.1016/j.ajur.2017.01.004.
doi: 10.1016/j.ajur.2017.01.004 pmid: 29387556 |
| 15. |
Hu H, Yao X, Xie X, et al. Prognostic value of preoperative NLR, dNLR, PLR and CRP in surgical renal cell carcinoma patients. World J Urol 2017; 35(2):261-70. doi: 10.1007/s00345-016-1864-9.
doi: 10.1007/s00345-016-1864-9 pmid: 27255479 |
| 16. | Cao ZP, Guan B, Zhao GZ, et al. Validation of the pretreatment neutrophil-to-lymphocyte ratio as a prognostic factor in a large cohort of Chinese patients with upper tract urothelial carcinoma. Chin Med J (Engl) 2017; 130(17):2063-8. doi: 10.4103/0366-6999.213414. |
| 17. |
Gu L, Ma X, Li H, et al. Prognostic value of preoperative inflammatory response biomarkers in patients with sarcomatoid renal cell carcinoma and the establishment of a nomogram. Sci Rep 2016; 6:23846. doi: 10.1038/srep23846.
doi: 10.1038/srep23846 pmid: 27035802 |
| 18. |
Cheng YC, Huang CN, Wu WJ, et al. The prognostic significance of inflammation-associated blood cell markers in patients with upper tract urothelial carcinoma. Ann Surg Oncol 2016; 23(1):343-51. doi: 10.1245/s10434-015-4781-z.
doi: 10.1245/s10434-015-4781-z pmid: 26242371 |
| 19. |
Byun SS, Hwang EC, Kang SH, et al. Prognostic significance of preoperative neutrophil-to-Lymphocyte ratio in nonmetastatic renal cell carcinoma: a large, multicenter cohort analysis. Biomed Res Int 2016; 2016:5634148. doi: 10.1155/2016/5634148.
doi: 10.1155/2016/5634148 pmid: 27891517 |
| 20. |
Wen RM, Zhang YJ, Ma S, et al. Preoperative neutrophil to lymphocyte ratio as a prognostic factor in patients with non-metastatic renal cell carcinoma. Asian Pac J Cancer Prev 2015; 16(9):3703-8. doi: 10.7314/apjcp.2015.16.9.3703.
pmid: 25987025 |
| 21. |
Tanaka N, Kikuchi E, Kanao K, et al. A multi-institutional validation of the prognostic value of the neutrophil-to-lymphocyte ratio for upper tract urothelial carcinoma treated with radical nephroureterectomy. Ann Surg Oncol 2014; 21(12):4041-8. doi: 10.1245/s10434-014-3830-3.
pmid: 24912614 |
| 22. |
Luo HL, Chen YT, Chuang YC, et al. Subclassification of upper urinary tract urothelial carcinoma by the neutrophil-to-lymphocyte ratio (NLR) improves prediction of oncological outcome. BJU Int 2014; 113(5b):E144-9. doi: 10.1111/bju.12582.
doi: 10.1111/bju.12582 pmid: 24274691 |
| 23. |
Dalpiaz O, Ehrlich GC, Mannweiler S, et al. Validation of pretreatment neutrophil-lymphocyte ratio as a prognostic factor in a European cohort of patients with upper tract urothelial carcinoma. BJU Int 2014; 114(3):334-9. doi: 10.1111/bju.12441.
doi: 10.1111/bju.12441 |
| 24. |
Pichler M, Hutterer GC, Stoeckigt C, et al. Validation of the pre-treatment neutrophil-lymphocyte ratio as a prognostic factor in a large European cohort of renal cell carcinoma patients. Br J Cancer 2013; 108(4):901-7. doi: 10.1038/bjc.2013.28.
pmid: 23385728 |
| 25. |
Azuma T, Matayoshi Y, Odani K, et al. Preoperative neutrophil-lymphocyte ratio as an independent prognostic marker for patients with upper urinary tract urothelial carcinoma. Clin Genitourin Cancer 2013; 11(3):337-41. doi: 10.1016/j.clgc.2013.04.003.
doi: 10.1016/j.clgc.2013.04.003 pmid: 23665132 |
| 26. |
Viers BR, Boorjian SA, Frank I, et al. Pretreatment neutrophil-to-lymphocyte ratio is associated with advanced pathologic tumor stage and increased cancer-specific mortality among patients with urothelial carcinoma of the bladder undergoing radical cystectomy. Eur Urol 2014; 66(6):1157-64. doi: 10.1016/j.eururo.2014.02.042.
doi: 10.1016/j.eururo.2014.02.042 |
| 27. |
Cho H, Hur HW, Kim SW, et al. Pre-treatment neutrophil to lymphocyte ratio is elevated in epithelial ovarian cancer and predicts survival after treatment. Cancer Immunol Immunother 2009; 58(1):15-23. doi: 10.1007/s00262-008-0516-3.
doi: 10.1007/s00262-008-0516-3 pmid: 18414853 |
| 28. |
Fondevila C, Metges JP, Fuster J, et al. p53 and VEGF expression are independent predictors of tumour recurrence and survival following curative resection of gastric cancer. Br J Cancer 2004; 90(1):206-15. doi: 10.1038/sj.bjc.6601455.
doi: 10.1038/sj.bjc.6601455 pmid: 14710231 |
| 29. |
Hwang GI, Yoo CH, Sohn BH, et al. Predictive value of preoperative serum CEA, CA19-9 and CA125 levels for peritoneal metastasis in patients with gastric carcinoma. Cancer Res Treat 2004; 36(3):178-81. doi: 10.4143/crt.2004.36.3.178.
doi: 10.4143/crt.2004.36.3.178 pmid: 20396541 |
| [1] | 沈畅, 赵萌, 李芸云, 刘宁朴. 荟萃分析:亚甲基四氢叶酸还原酶基因C677T(MTHFR-C677T)多态性与糖尿病视网膜病变(DR)的关系[J]. Chinese Medical Sciences Journal, 2020, 35(1): 71-84. |
| 阅读次数 | ||||||
|
全文 |
|
|||||
|
摘要 |
|
|||||
|