Chinese Medical Sciences Journal ›› 2022, Vol. 37 ›› Issue (4): 287-292.doi: 10.24920/004130
• Original Articles • Next Articles
Risk Factors for Anesthesia-Related Airway Patient Safety Incidents: A Single-Center Retrospective Case-Control Analysis from 2009 to 2022
Xue Zhang1, Lingeer Wu1, Huizhen Huang1, Yuelun Zhang2, Zhilong Lu1, Yajie Tian1, Le Shen1, *( ), Yuguang Huang1
), Yuguang Huang1
- 1Department of Anesthesiology, Beijing 100730, China
2Medical Research Center;Peking Union Medical College Hospital, Chinese Academy of Medical Sciences & Peking Union Medical College, Beijing 100730, China
-
Received:2022-06-23Accepted:2022-09-30Published:2022-12-31Online:2022-10-10 -
Contact:Le Shen E-mail:pumchshenle@163.com
Cite this article
Xue Zhang, Lingeer Wu, Huizhen Huang, Yuelun Zhang, Zhilong Lu, Yajie Tian, Le Shen, Yuguang Huang. Risk Factors for Anesthesia-Related Airway Patient Safety Incidents: A Single-Center Retrospective Case-Control Analysis from 2009 to 2022[J].Chinese Medical Sciences Journal, 2022, 37(4): 287-292.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
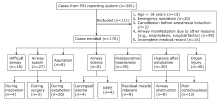
Figure 1.
Enrollment and classification of airway-related PSIs. This figure shows the classification of airway-related PSIs reported by anesthesiologists during September 2009 to May 2022 as well as the number of cases in each category. PSI: patient safety incident; NPPE: negative pressure pulmonary edema."
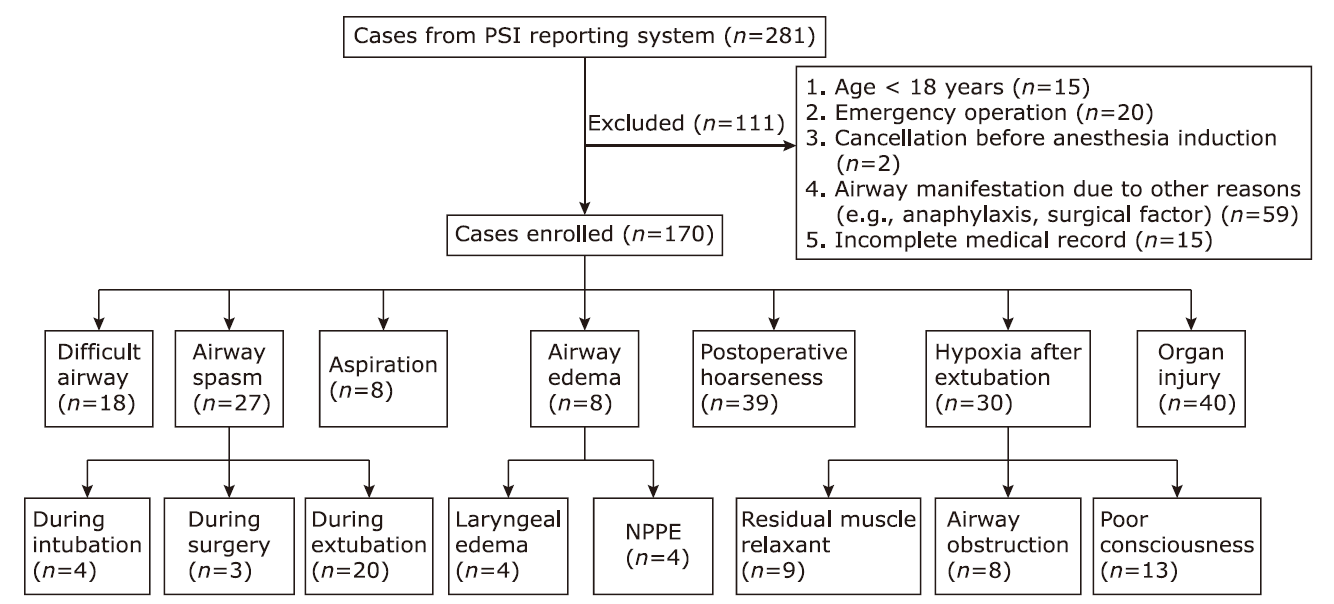
Table 1.
Risk factors associated with airway-related PSI occurrence found via univariable analysis"
| Risk factors | Airway PSI group (n = 170) | Control group (n = 170) | Mean difference/OR (95%CI) | P value |
|---|---|---|---|---|
| Age (yrs, mean±SD) | 54.63±??.49 | 52.63±??.52 | 2.00 (-1.10 to 5.10) | 0.206 |
| Height (cm, mean±SD) | 165.27±8.62 | 165.80±?.47 | -0.53 (-2.29 to 1.24) | 0.559 |
| Weight (kg, mean±SD) | 66.13±3.19 | 64.75±?1.72 | 1.38 (-1.29 to 4.04) | 0.310 |
| BMI (kg/m2, mean±SD) | 24.09±?.25 | 23.54±?.41 | 0.55 (-0.29 to 1.40) | 0.197 |
| ASA PS (n) | ||||
| Ⅰ | 24 | 46 | Reference | |
| Ⅱ | 112 | 110 | 1.59 (0.86 to 2.93) | 0.137 |
| Ⅲ | 34 | 14 | 3.40 (1.42 to 8.11) | 0.006 |
| Preoperative comorbidities (n) | ||||
| Hypertension | 53 | 38 | 1.57 (0.97 to 2.56) | 0.066 |
| Diabetes | 26 | 18 | 1.53 (0.80 to 2.90) | 0.196 |
| Smoking history (n) | 44 | 42 | 1.06 (0.65 to 1.74) | 0.803 |
| Drinking history (n) | 25 | 25 | 1.00 (0.55 to 1.82) | 1.000 |
| Preoperative laboratory test indices (mean±SD) | ||||
| WBC (×109/L) | 6.55±1.96 | 6.52±2.47 | 0.03 (-0.45 to 0.50) | 0.906 |
| NEUT (%) | 62.03±10.39 | 61.06±10.64 | 0.97 (-1.28 to 3.22) | 0.396 |
| LY (%) | 28.12±9.32 | 29.23±9.42 | -1.11 (-3.11 to 0.89) | 0.276 |
| HGB (g/L) | 132.19±25.22 | 135.65±18.54 | -3.46 (-8.19 to 1.28) | 0.152 |
| Hct (%) | 39.84±5.51 | 40.27±4.97 | -0.43 (-1.56 to 0.69) | 0.446 |
| PLT (×109/L) | 241.13±80.60 | 240.30±70.94 | 0.83 (-15.40 to 17.06) | 0.920 |
| ALT (U/L) | 30.90±49.79 | 27.17±47.00 | 3.73 (-6.62 to 14.07) | 0.479 |
| Alb (g/L) | 41.65±4.96 | 42.98±3.96 | -1.32 (-2.29 to -0.36) | 0.007 |
| Serum Cr (μmol/L) | 69.10±21.48 | 67.50±15.94 | 1.60 (-2.44 to 5.65) | 0.437 |
| PT (s) | 11.83±0.99 | 11.64±1.14 | 0.18 (-0.04 to 0.41) | 0.114 |
| APTT (s) | 27.96±3.96 | 27.05±3.25 | 1.03 (-0.01 to 2.07) | 0.051 |
| Fibrinogen (g/L) | 3.28±1.26 | 2.99±0.89 | 0.29 (0.05 to 0.52) | 0.016 |
| Glucose (mmol/L) | 5.70±1.28 | 5.64±1.50 | 0.05 (-0.25 to 0.35) | 0.722 |
Table 2.
Risk factors associated with airway-related PSI occurrence identified via multivariable analysis"
| Groups | ASA PS (n) | Age (yrs) | Alb (g/L) | Fibrinogen (g/L) | BMI (kg/m2) | Hypertension (n) | ||
|---|---|---|---|---|---|---|---|---|
| Ⅰ | Ⅱ | Ⅲ | ||||||
| Control group | 46 | 110 | 14 | 52.63±13.52 | 42.98±3.96 | 2.99±0.89 | 23.54±3.41 | 38 |
| Airway PSI group | 24 | 112 | 34 | 54.63±15.49 | 41.65±4.96 | 3.28±1.26 | 24.09±4.25 | 53 |
| OR (95%CI) | Reference | 1.65 (0.88 to 3.08) | 3.50 (1.45 to 8.42) | 1.00 (0.98 to 1.01) | 0.97 (0.91 to 1.02) | 1.16 (0.92 to 1.47) | 1.04 (0.98 to 1.11) | 1.16 (0.66 to 2.05) |
| P value | 0.020 | 0.627 | 0.208 | 0.213 | 0.202 | 0.603 | ||
Table 3.
Prognosis of patients with airway incidents (n = 170)"
| Groups | Extubation time (d, mean±SD) | ICU LOS (d, mean±SD) | Post-operative LOS (d, mean±SD) | In-hospital LOS (d, mean±SD) | Complications (n) | |
|---|---|---|---|---|---|---|
| Pulmonary infection | MACE | |||||
| Control group | 0.16±0.77 | 0.19±0.84 | 7.59±10.76 | 11.62±11.88 | 4 | 1 |
| Airway PSI group | 0.72±1.56 | 1.63±5.71 | 10.56±13.09 | 14.99±15.18 | 11 | 7 |
| Mean difference/OR (95%CI) | 0.55 (0.29 to 0.82) | 1.44 (0.57 to 2.32) | 2.97 (0.41 to 5.53) | 3.37 (0.46 to 6.27) | 2.87 (0.90 to 9.020) | 7.26 (0.88 to 59.64) |
| P value | < 0.001 | 0.001 | 0.023 | 0.024 | 0.065 | 0.067 |
| [1] | World Health Organization. ‘More than words’—conceptual framework for the international classification for patient safety. Geneva: World Health Organization; 2009. |
| [2] |
Zhang X, Ma S, Sun X, et al. Composition and risk assessment of perioperative patient safety incidents reported by anesthesiologists from 2009 to 2019: a single-center retrospective cohort study. BMC Anesth 2021; 21 (1): 8. doi: 10.1186/s12871-020-01226-0.
doi: 10.1186/s12871-020-01226-0 |
| [3] |
Saito T, Wong ZW, Thinn KK, et al. Review of critical incidents in a university department of anaesthesia. Anesth Intensive Care 2015; 43(2):238-43. doi: 10.1177/0310057X1504300215.
doi: 10.1177/0310057X1504300215 |
| [4] |
Thomas AN, Taylor RJ. Review of patient safety incidents reported from 541 critical care units in North-West England in 2009 and 2010. Anaesthesia 2012; 67(7):706-13. doi: 10.1111/j.1365-2044.2012.07141.x.
doi: 10.1111/j.1365-2044.2012.07141.x pmid: 22506637 |
| [5] |
Thomas AN, McGrath BA. Patient safety incidents associated with airway devices in critical care: a review of reports to the UK National Patient Safety Agency. Anesthesia 2009; 64(4):358-65. doi: 10.1111/j.1365-2044.2008.05784.x.
doi: 10.1111/j.1365-2044.2008.05784.x |
| [6] |
Cook TM, Woodall N, Harper J, et al. Fourth National Audit Project. Major complications of airway management in the UK: results of the Fourth National Audit Project of the Royal College of Anaesthetists and the Difficult Airway Society. Part 2: intensive care and emergency departments. Br J Anesth 2011; 106(5):632-42. doi: 10.1093/bja/aer059.
doi: 10.1093/bja/aer059 |
| [7] |
Alonso-Ovies Á, Nin N, Martín MC, et al. Safety incidents in airway and mechanical ventilation in Spanish ICUs: the IVeMVA study. J Crit Care 2018; 47:238-44. doi: 10.1016/j.jcrc.2018.07.012.
doi: S0883-9441(18)30321-6 pmid: 30056219 |
| [8] |
Mitchell I, Schuster A, Smith K, et al. Patient safety incident reporting: a qualitative study of thoughts and perceptions of experts 15 years after ‘To Err is Human’. BMJ Qual Saf 2016; 25(2):92-9. doi: 10.1136/bmjqs-2015-004405.
doi: 10.1136/bmjqs-2015-004405 pmid: 26217037 |
| [9] |
Mahajan RP. Critical incident reporting and learning. Br J Anesth 2010; 105(1):69-75. doi: 10.1093/bja/aeq133.
doi: 10.1093/bja/aeq133 |
| [10] |
Wallace LM, Spurgeon P, Benn J, et al. Improving patient safety incident reporting systems by focusing upon feedback-lessons from English and Welsh trusts. Health Serv Manage Res 2009; 22(3):129-35. doi: 10.1258/hsmr.2008.008019.
doi: 10.1258/hsmr.2008.008019 |
| [11] |
Frerk C, Mitchell VS, McNarry AF, et al. Difficult Airway Society 2015 guidelines for management of unanticipated difficult intubation in adults. Br J Anesth 2015; 115(6):827-48. doi: 10.1093/bja/aev371.
doi: 10.1093/bja/aev371 |
| [12] |
Kornas RL, Owyang CG, Sakles JC, et al. Evaluation and management of the physiologically difficult airway: consensus recommendations from Society for Airway Management. Anesth Analg 2021; 132(2):395-405. doi: 10.1213/ANE.0000000000005233.
doi: 10.1213/ANE.0000000000005233 pmid: 33060492 |
| [13] |
Apfelbaum JL, Hagberg CA, Connis RT, et al. 2022 American Society of Anesthesiologists Practice Guidelines for Management of the Difficult Airway. Anesthesiology 2022 ; 136(1):31-81. doi: 10.1097/ALN.0000000000004002.
doi: 10.1097/ALN.0000000000004002 |
| [14] |
Kaiser HA, Saied NN, Kokoefer AS, et al. Incidence and prediction of intraoperative and postoperative cardiac arrest requiring cardiopulmonary resuscitation and 30-day mortality in non-cardiac surgical patients. PLoS One 2020; 15(1): e0225939. doi: 10.1371/journal.pone.0225939.
doi: 10.1371/journal.pone.0225939 |
| [15] |
Sobreira-Fernandes D, Teixeira L, Lemos TS, et al. Perioperative cardiac arrests—a subanalysis of the anesthesia-related cardiac arrests and associated mortality. J Clin Anesth 2018; 50:78-90. doi: 10.1016/j.jclinane.2018.06.005.
doi: S0952-8180(18)30260-5 pmid: 30005296 |
| [16] |
Banik RK, Honeyfield K, Qureshi S, et al. Incidence and mortality rate of perioperative reintubation: case series of 196 patients. AANA J 2021; 89(6):476-9.
pmid: 34809752 |
| [17] |
Endlich Y, Beckmann LA, Choi SW, et al. A prospective six-month audit of airway incidents during anesthesia in twelve tertiary level hospitals across Australia and New Zealand. Anesth Intensive Care 2020; 48(5):389-98. doi: 10.1177/0310057X20945325.
doi: 10.1177/0310057X20945325 |
| [1] | Yu Gu, Ting Zhang, Min Peng, Juhong Shi. Characteristics and Prognosis of Microscopic Polyangiitis Patients with Diffuse Alveolar Hemorrhage and Interstitial Lung Disease [J]. Chinese Medical Sciences Journal, 2022, 37(4): 293-302. |
| [2] | Lulu Ma, Xuerong Yu, Xisheng Weng, Jin Lin, Jin Jin, Wenwei Qian, Yuguang Huang. Possible Risk Factors for Severe Complications Occurring after Primary Total Knee Arthroplasty [J]. Chinese Medical Sciences Journal, 2022, 37(4): 303-308. |
| [3] | Lijin Lin, Yemao Liu, Juanjuan Qin, Fang Lei, Wenxin Wang, Xuewei Huang, Weifang Liu, Xingyuan Zhang, Zhigang She, Peng Zhang, Xiaojing Zhang, Zhaoxia Jin, Hongliang Li. Global and Regional Trends and Projections of Infective Endocarditis-Associated Disease Burden and Attributable Risk Factors from 1990 to 2030 [J]. Chinese Medical Sciences Journal, 2022, 37(3): 181-194. |
| [4] | Junxiong Yin, Cheng Yu, Lixia Wei, Chuanyong Yu, Hongxing Liu, Mingyang Du, Feng Sun, Chongjun Wang, Xiaoshan Wang. Detection of Asymptomatic Carotid Artery Stenosis in High-Risk Individuals of Stroke Using a Machine-Learning Algorithm [J]. Chinese Medical Sciences Journal, 2020, 35(4): 297-305. |
| [5] | Zuo Mingzhang,Huang Yuguang,Ma Wuhua,Xue Zhanggang,Zhang Jiaqiang,Gong Yahong,Che Lu, Chinese Society of Anesthesiology Task Force on Airway Management. Expert Recommendations for Tracheal Intubation in Critically Ill Patients with Noval Coronavirus Disease 2019 [J]. Chinese Medical Sciences Journal, 2020, 35(2): 105-109. |
| [6] | Li Tao, Yang Li, Zhang Weiguo, Luo Chuncai, Huang Zili, Li Jinfeng, Li Xin. Midterm Follow-up of Coronary Artery Bypass Grafting with 64-Slice Multi-detector Computed Tomography: Identification of Risk Factors Affecting Graft Patency [J]. Chinese Medical Sciences Journal, 2018, 33(2): 69-76. |
| [7] | Rong Yuan, Jie Wang, Li-li Guo. The Effect of Sleep Deprivation on Coronary Heart Disease [J]. Chinese Medical Sciences Journal, 2016, 31(4): 247-253. |
| [8] | Dong Yang, Shi-yi Tong, Jin-hua Jin, Geng-zhi Tang, Jing-hu Sui, Ling-xin Wei, Xiao-ming Deng. Shikani Optical Stylet-guided Intubation via the Intubating Laryngeal Airway in Patients With Scar Contracture of the Face and Neck [J]. Chinese Medical Sciences Journal, 2013, 28(4): 195-200. |
| [9] | Xiao-dong Qu, Resha Shrestha and Mao-de Wang* . Risk Factors Analysis on Traumatic Brain Injury Prognosis [J]. Chinese Medical Sciences Journal, 2011, 26(2): 98-102. |
| [10] | Hai-ling Wang, Yu Wang, Ying Zhang, Yun-dai Chen, Xin-chun Wang, Zhi-xuan Liu, Guo-li Jing, Hai-feng Tong, Yuan Tian, and Qing-zeng Liu. Changes in Plasma Angiotensin II and Circadian Rhythm of Blood Pressure in Hypertensive Patients with Sleep Apnea Syndrome Before and After Treatment [J]. Chinese Medical Sciences Journal, 2011, 26(1): 9-13. |
| [11] | Song Fu, Zhi-cun Feng and Schranz Dietmar. Factors Influencing Pleural Effusion after Fontan Operation:an Analysis with 95 Patients [J]. Chinese Medical Sciences Journal, 2010, 25(1): 38-43. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||
|

