Chinese Medical Sciences Journal ›› 2024, Vol. 39 ›› Issue (1): 54-68.doi: 10.24920/004294
右美托咪定对脊柱手术患者术中血流动力学和失血量的影响:系统回顾和荟萃分析
- 1麻醉科,中国人民解放军联勤保障部队第925医院,贵阳 550000,中国
2骨科,中国人民解放军联勤保障部队第925医院,贵阳 550000,中国
-
收稿日期:2023-08-23接受日期:2024-01-22出版日期:2024-03-31发布日期:2024-03-01 -
通讯作者:瞿金涛
Effect of Dexmedetomidine on Intraoperative Hemodynamics and Blood Loss in Patients Undergoing Spine Surgery: A Systematic Review and Meta-Analysis
Mei Wang1,Jian-Xiang Che1,Lei Chen1,Ting-Ting Song1,Jin-Tao Qu2,*( )
)
- 1Department of Anesthesiology, The 925th Hospital of People's Liberation Army (PLA) Joint Logistics Support Force, Guiyang, Guizhou 550000, China
2Department of Orthopedics, The 925th Hospital of People's Liberation Army (PLA) Joint Logistics Support Force, Guiyang, Guizhou 550000, China
-
Received:2023-08-23Accepted:2024-01-22Published:2024-03-31Online:2024-03-01 -
Contact:* Jin-Tao Qu, E-mail:qu_jintao@126.com .
摘要:
目的 右美托咪定是一种高选择性的α2肾上腺素能受体激动剂,具有降低血压和心率的作用。本研究旨在探讨右美托咪定对脊柱手术患者术中血流动力学和失血量的影响。
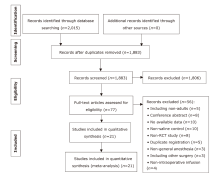
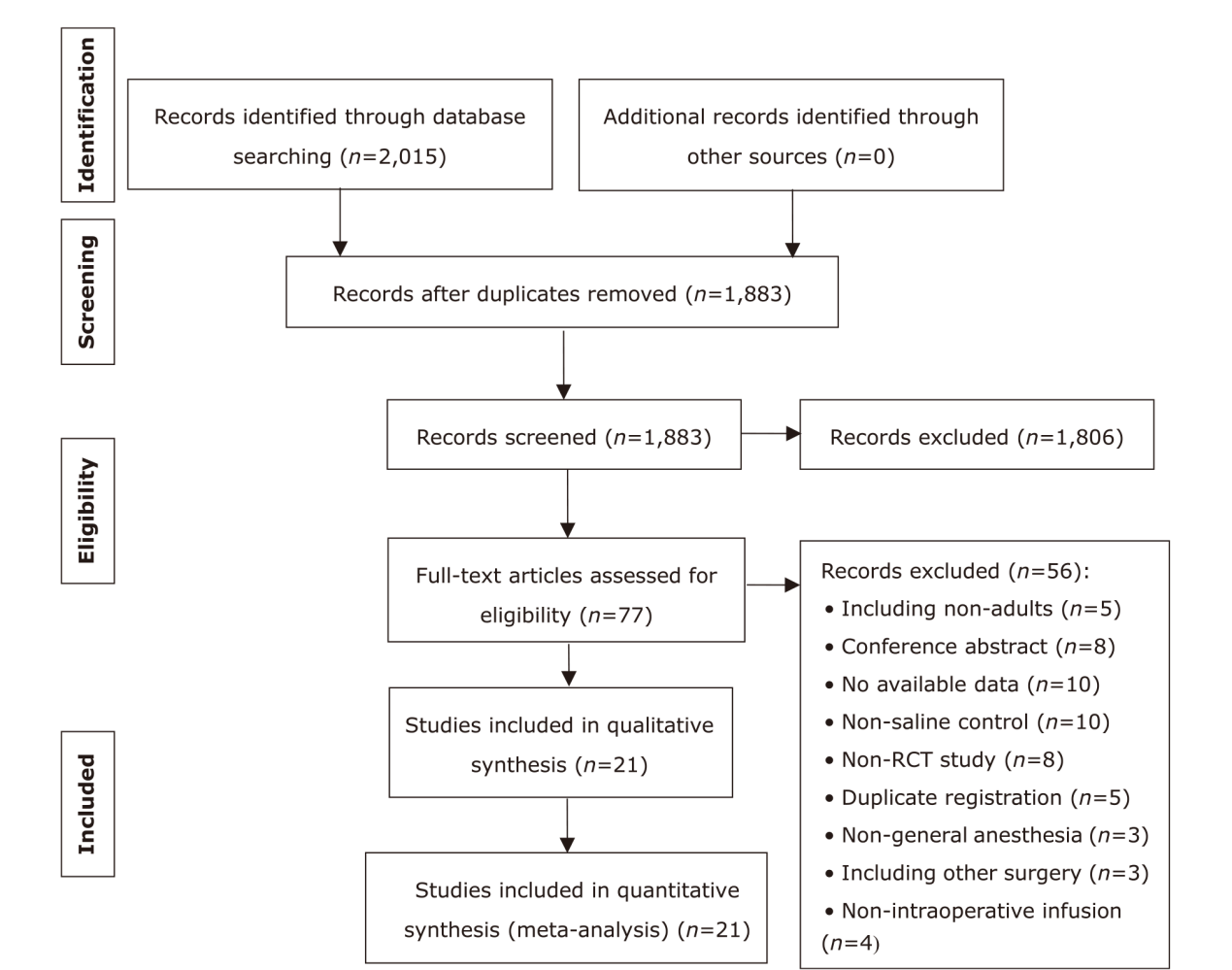
方法 检索Web of Science、MEDLINE、EMBASE和Cochrane图书馆截至2023年2月发表的随机对照研究,比较右美托咪定和生理盐水对脊柱手术术中血流动力学和失血量的影响。根据研究间的异质性采用固定或随机效应模型。
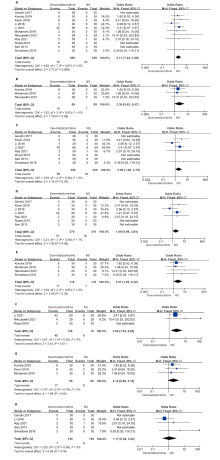
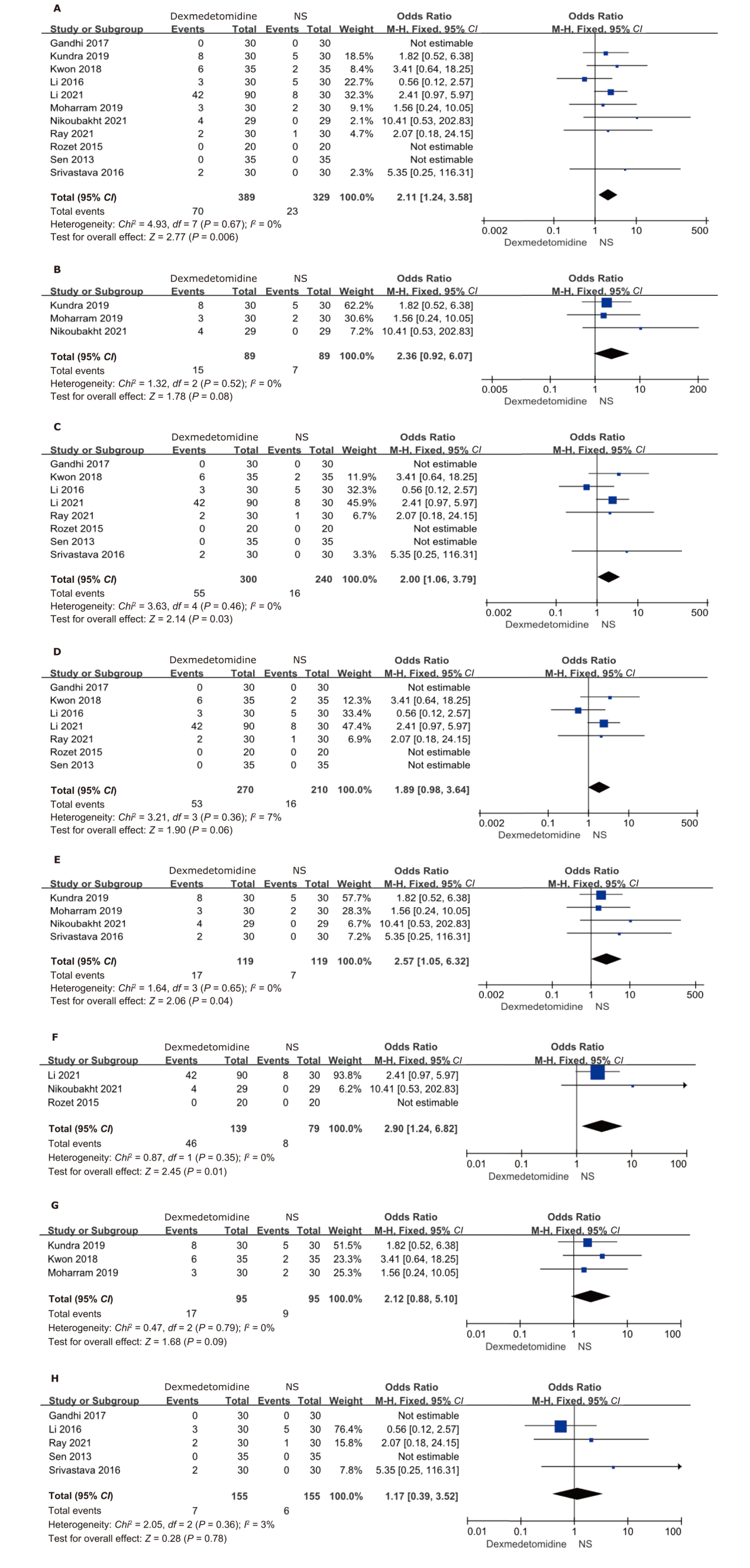
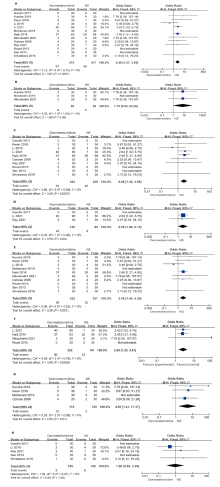
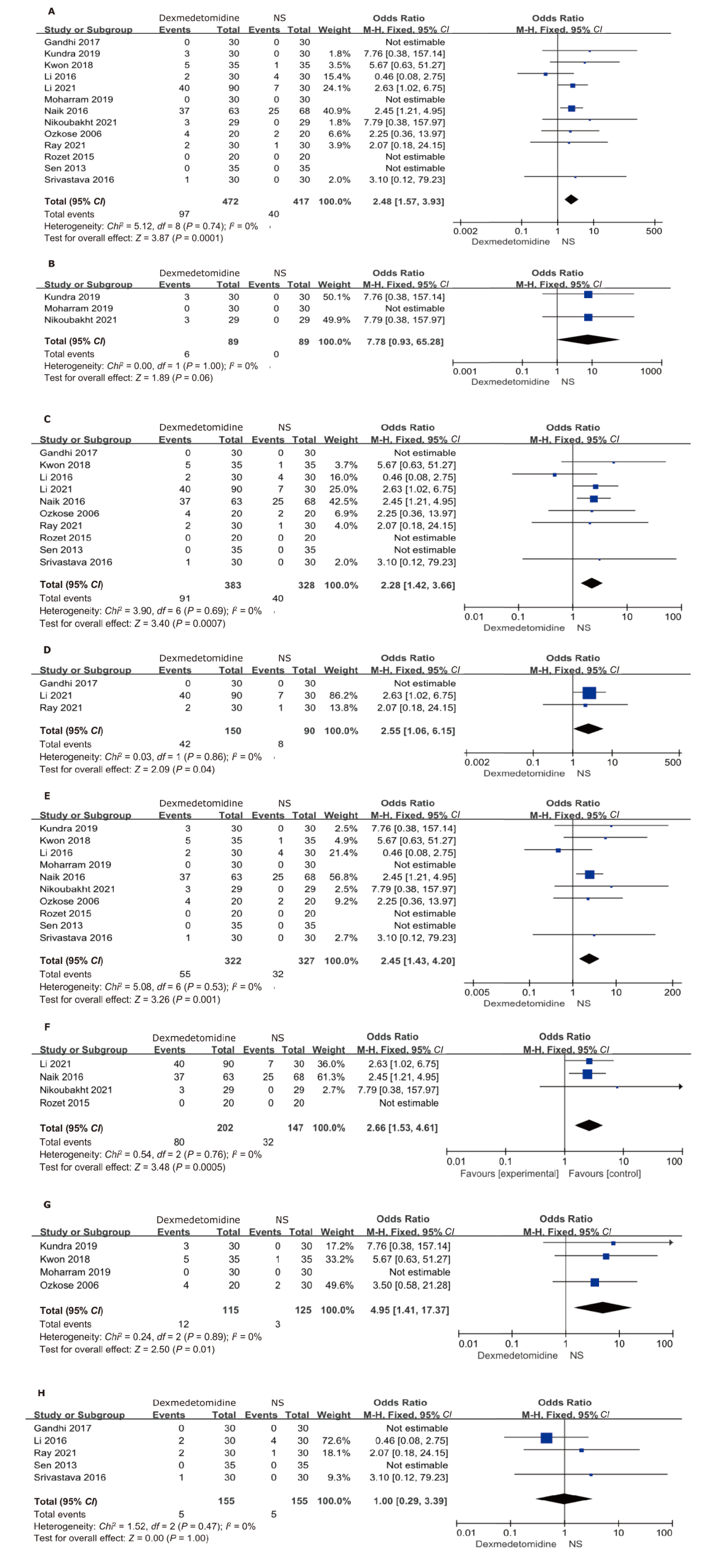
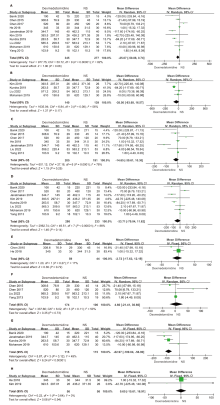
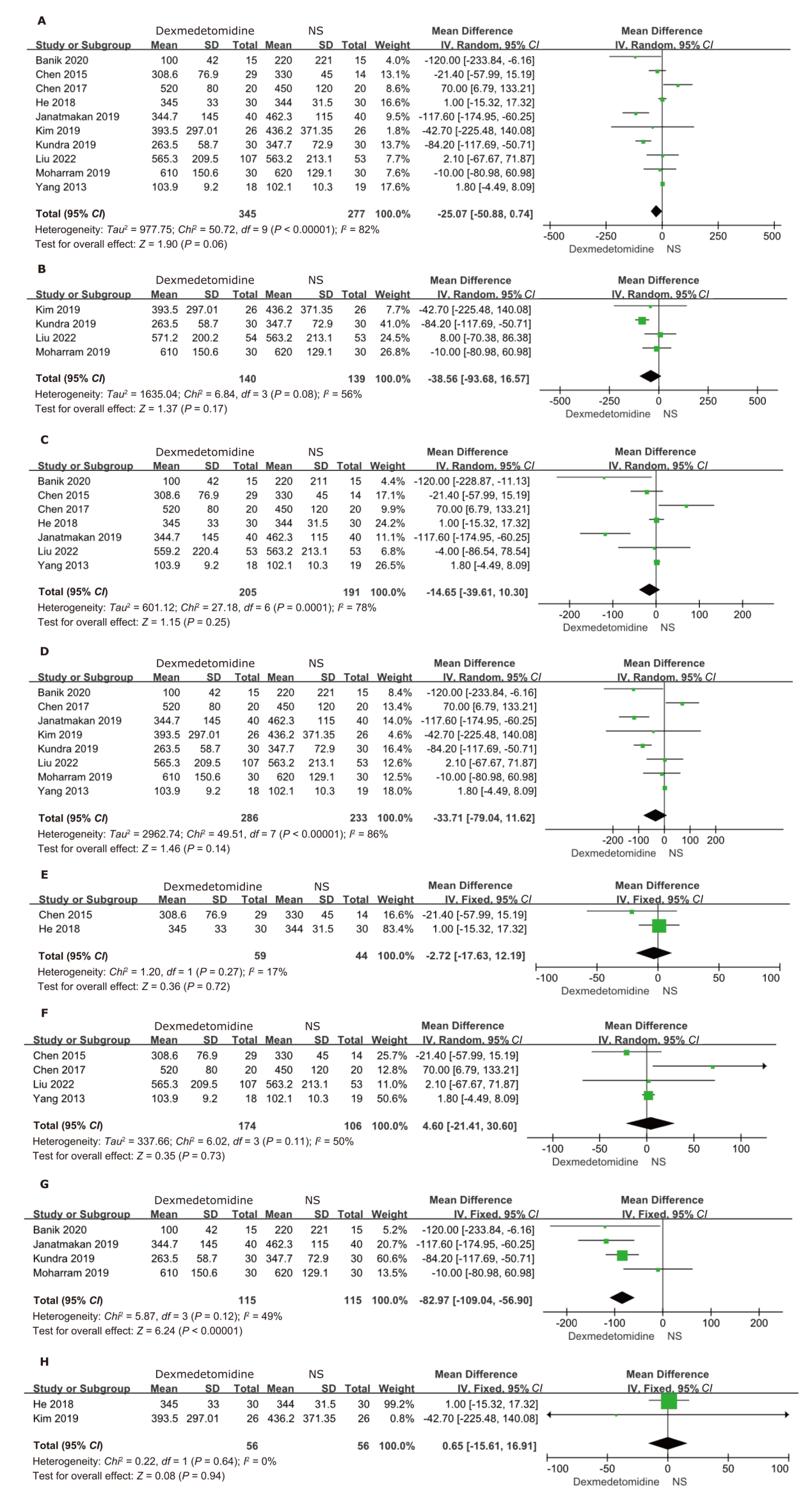
结果 纳入21项随机对照研究,共1388例患者。右美托咪定的使用增加了术中低血压(OR:2.11;95%CI:1.24 - 3.58;P=0.006)和心动过缓(OR:2.48;95%CI:1.57 - 3.93;P=0.0001)的总体风险。特别是在给予负荷剂量时,低血压(OR:2.00;95%CI:1.06 - 3.79;P=0.03)和心动过缓(OR:2.28;95%CI:1.42 - 3.66;P=0.0007)的风险更为显著。当右美托咪定与静脉麻醉联合使用时,患者更容易出现血流动力学不稳定的情况,包括低血压(OR:2.90;95%CI:1.24 - 6.82;P=0.01)和心动过缓(OR:2.66;95%CI:1.53 - 4.61;P=0.0005)。与吸入麻醉联合时,仅增加了心动过缓的风险(OR:4.95;95%CI:1.41 - 17.37;P=0.01)。然而,当与静吸复合麻醉联合使用时,并未增加低血压和心动过缓的风险。此外,右美托咪定还增加了重度低血压的风险(OR:2.57;95%CI:1.05 - 6.32;P=0.04),但对轻度低血压的影响并不显著。对于心动过缓而言,无论是轻度(OR:2.55;95%CI:1.06-6.15;P=0.04)还是重度(OR:2.45;95%CI:1.43 - 4.20;P=0.001)的风险都有所增加。总体而言,右美托咪定对术中失血量的影响并不显著,但在与吸入麻醉联合时,失血量显著减少(MD:-82.97;95%CI:-109.04 - -56.90;P<0.001)。
结论 右美托咪定在脊柱手术过程中增加了低血压和心动过缓的风险。给予负荷剂量或与不同麻醉维持方式联合使用可能会对术中血流动力学和失血量产生不同的影响。然而,目前的研究结果仍需进一步证实和探讨。
引用本文
Mei Wang, Jian-Xiang Che, Lei Chen, Ting-Ting Song, Jin-Tao Qu. Effect of Dexmedetomidine on Intraoperative Hemodynamics and Blood Loss in Patients Undergoing Spine Surgery: A Systematic Review and Meta-Analysis[J].Chinese Medical Sciences Journal, 2024, 39(1): 54-68.
"
| Author year | Country | Age range (ys) | Sample size (n) | Intervention | Outcome measures | Surgery type | |
|---|---|---|---|---|---|---|---|
| Dex | Saline | ||||||
| Li 2016 | China | 18 — 65 | 30 | 30 | Loading dose of 0.5μg·kg-1 for 10min; maintenance dose of 0.2μg·kg-1·h-1 | ①② | Major spine surgery |
| Li 2021* | China | 65 — 90 | D1: 30 D2: 30 D3: 30 | 30 | D1: Loading dose of 0.3μg·kg-1 for 10min; maintenance dose of 0.2μg·kg-1·h-1 D2: Loading dose of 0.3μg·kg-1 for 10min; maintenance dose of 0.5μg·kg-1·h-1 D3: Loading dose of 0.3μg·kg-1 for 10min; maintenance dose of 0.8μg·kg-1·h-1 | ①② | Spine surgery |
| Sen 2013 | India | 20 — 60 | 35 | 35 | Loading dose of 1μg·kg-1 for 10min; maintenance dose of 0.2μg·kg-1·h-1 | ①② | Spine surgery |
| Naik 2016 | USA | 18 — 80 | 63 | 68 | Loading dose of 1μg·kg-1 for 20min; maintenance dose of 0.5μg·kg-1·h-1 | ② | Thoracic and lumbar spine surgery |
| Kim 2019 | Korea | 20 — 70 | 26 | 26 | Maintenance dose of 0.4μg·kg-1·h-1 | ③ | Spine fusion surgery |
| Gandhi 2017 | India | 18 — 60 | 30 | 30 | Loading dose of 1μg·kg-1 for 10min; maintenance dose of 0.5μg·kg-1·h-1 | ①② | Cervical spine surgery |
| Kwon 2018 | Korea | 20 — 65 | 35 | 35 | Loading dose of 1μg·kg-1 for 10min; maintenance dose of 0.3-0.5μg·kg-1·h-1 | ①② | Lumbar microdiscectomy |
| Chen 2017 | China | 18 — 60 | 20 | 20 | Loading dose of 0.5μg·kg-1 for 10min; maintenance dose of 0.2μg·kg-1·h-1 | ③ | Posterior thoracolumbar surgery |
| Ozkose 2006 | Turkey | ≥18 | 20 | 20 | Loading dose of 1μg·kg-1 for 10min; maintenance dose of 0.2μg·kg-1·h-1 | ② | Lumbar spine surgery |
| Chen 2015* | China | 65 — 80 | D1: 14 D2: 15 | 14 | D1: Loading dose of 0.3μg·kg-1 for 10min; maintenance dose of 0.3μg·kg-1·h-1 D2: Loading dose of 0.8μg·kg-1 for 10min; maintenance dose of 0.8μg·kg-1·h-1 | ③ | Spine surgery |
| Banik 2020 | India | 18 — 60 | 15 | 15 | Loading dose of 1μg·kg-1 for 10min; maintenance dose of 0.5μg·kg-1·h-1 | ③ | Lumbar spine surgery |
| Kundra 2019 | India | 18 — 65 | 30 | 30 | Maintenance dose of 0.3μg·kg-1·h-1 | ①②③ | Lumbar spine surgery |
| Rozet 2015 | USA | ≥18 | 20 | 20 | Loading dose of 0.6μg·kg-1 for 10min; maintenance dose of 0.6μg·kg-1·h-1 | ①② | Spine surgery |
| Janatmakan 2019 | Iran | 20 — 50 | 38 | 39 | Loading dose of 0.5μg·kg-1 for 10min; maintenance dose of 0.25μg·kg-1·h-1 | ③ | Spine surgery |
| Srivastava 2016 | India | 20 — 60 | 30 | 30 | Loading dose of 1μg·kg-1 for 15min; maintenance dose of 0.5μg·kg-1·h-1 | ①② | Spine surgery |
| Yang 2013 | China | 40 — 60 | 18 | 19 | Loading dose of 0.7μg·kg-1 for 15min; maintenance dose of 0.6μg·kg-1·h-1 | ③ | Lumbar discectomy |
| Moharram 2019 | Egypt | 18 — 65 | 30 | 30 | Maintenance dose of 0.5μg·kg-1·h-1 | ①②③ | Lumbar spine instrumentation surgery |
| He 2018 | China | 75 — 90 | 30 | 30 | Loading dose of 0.5μg·kg-1 for 10min; maintenance dose of 0.4μg·kg-1·h-1 | ③ | Thoracic or lumbar fracture surgery |
| Nikoubakht 2021 | Iran | 18 — 70 | 29 | 29 | Maintenance dose of 0.2μg·kg-1·h-1 | ①② | Posterior spine fusion |
| Ray 2021 | India | 30 — 60 | 30 | 30 | Loading dose of 1μg·kg-1 for 10min; maintenance dose of 0.5μg·kg-1·h-1 | ①② | Spine surgery |
| Liu 2022* | China | 18 — 60 | D1: 53 D2: 54 | 53 | D1: Maintenance dose of 0.5μg·kg-1·h-1 D2: Loading dose of 1μg·kg-1 for 10min; maintenance dose of 0.5μg·kg-1·h-1 | ① | Thoracic spinal decompression surgery |
| 1. | Leigh JM. The history of controlled hypotension. Br J Anaesth 1975; 47(7): 745-9. doi: 10.1093/bja/47.7.745. |
| 2. | Degoute CS. Controlled hypotension: a guide to drug choice. Drugs 2007; 67(7): 1053-76. doi: 10.2165/00003495-200767070-00007. |
| 3. |
Weerink M, Struys M, Hannivoort LN, et al. Clinical pharmacokinetics and pharmacodynamics of dexmedetomidine. Clin Pharmacokinet 2017; 56(8): 893-913. doi: 10.1007/s40262-017-0507-7.
pmid: 28105598 |
| 4. | Tian LJ, Yao YT, Yuan S, et al. Effect of dexmedetomidine on maintaining perioperative hemodynamic stability in elderly patients: a systematic review and meta-analysis. Chin Med Sci J 2023; 38(1): 1-10. doi: 10.24920/004088. |
| 5. |
Wan X, Wang W, Liu J, et al. Estimating the sample mean and standard deviation from the sample size, median, range and/or interquartile range. BMC Med Res Methodol 2014; 14: 135. doi: 10.1186/1471-2288-14-135.
pmid: 25524443 |
| 6. | Rao G, Lopez-Jimenez F, Boyd J, et al. Methodological standards for meta-analyses and qualitative systematic reviews of cardiac prevention and treatment studies: a scientific statement from the American Heart Association. Circulation 2017; 136(10): e172-172e194. doi: 10.1161/CIR.0000000000000523. |
| 7. | Higgins JPT, Deeks JJ, Altman DG. Chapter 16:Special Topics In Statistics, Cochrane Handbook for Systematic Reviews of Interventions. JPT Higgins and JJ Deeks, eds. Sussex, England: The Cochrane Collaboration, 2011, pp 481-530. |
| 8. |
Higgins JP, Thompson SG. Quantifying heterogeneity in a meta-analysis. Stat Med 2002; 21(11): 1539-58. doi: 10.1002/sim.1186.
pmid: 12111919 |
| 9. |
Egger M, Davey Smith G, Schneider M, et al. Bias in meta-analysis detected by a simple, graphical test. BMJ 1997; 315(7109): 629-34. doi: 10.1136/bmj.315.7109.629.
pmid: 9310563 |
| 10. | Li Z, Li H, Yao S, et al. [Effects of dexmedetomidine doses on postoperative cognitive dysfunction and serum β- amyloid and cytokine levels in elderly patients after spine surgery: a randomized controlled trial]. Nan Fang Yi Ke Da Xue Xue Bao 2021; 41(4): 600-6. (Chinese) doi: 10.12122/j.issn.1673-4254.2021.04.18. |
| 11. | Chen Z, Lin S, Shao W. Effects on somatosensory and motor evoked potentials of senile patients using different doses of dexmedetomidine during spine surgery. Ir J Med Sci 2015; 184(4): 813-8. doi: 10.1007/s11845-014-1178-0. |
| 12. | He F, Shen L, Zhong J. A study of dexmedetomidine in the prevention of postoperative delirium in elderly patients after vertebral osteotomy. Int J Clin Exp Med 2018; 11(5): 4984-90. |
| 13. | Li BY, Geng ZY, Wang DX. [Effect of dexmedetomidine infusion on postoperative recovery for patients undergoing major spinal surgery during propofol anesthesia]. Beijing Da Xue Xue Bao Yi Xue Ban 2016; 48(3): 529-33. (Chinese) |
| 14. |
Sen S, Chakraborty J, Santra S, et al. The effect of dexmedetomidine infusion on propofol requirement for maintenance of optimum depth of anaesthesia during elective spine surgery. Indian J Anaesth 2013; 57(4): 358-63. doi: 10.4103/0019-5049.118558.
pmid: 24163449 |
| 15. |
Naik BI, Nemergut EC, Kazemi A, et al. The effect of dexmedetomidine on postoperative opioid consumption and pain after major spine surgery. Anesth Analg 2016; 122(5): 1646-53. doi: 10.1213/ANE.0000000000001226.
pmid: 27003917 |
| 16. | Gandhi KA, Panda NB, Vellaichamy A, et al. Intraoperative and postoperative administration of dexmedetomidine reduces anesthetic and postoperative analgesic requirements in patients undergoing cervical spine surgeries. J Neurosurg Anesthesiol 2017; 29(3): 258-63. doi: 10.1097/ANA.0000000000000301. |
| 17. |
Kwon Y, Jang JS, Hwang SM, et al. Intraoperative administration of dexmedetomidine reduced the postoperative catheter-related bladder discomfort and pain in patients undergoing lumbar microdiscectomy. J Anesth 2018; 32(1): 41-7. doi: 10.1007/s00540-017-2425-0.
pmid: 29098393 |
| 18. |
Chen Z, Dai N, Lin S, et al. Impact of dexmedetomidine on intraoperative wake-up tests in patients undergoing spinal surgery. J Perianesth Nurs 2018; 33(4): 448-52. doi: 10.1016/j.jopan.2016.07.009.
pmid: 30077288 |
| 19. | Ozkose Z, Demir FS, Pampal K, et al. Hemodynamic and anesthetic advantages of dexmedetomidine, an α2-agonist, for surgery in prone position. Tohoku J Exp Med 2006; 210(2): 153-60. doi: 10.1620/tjem.210.153. |
| 20. | Banik S, Rath GP, Lamsal R, et al. Effect of dexmedetomidine on dynamic cerebral autoregulation and carbon dioxide reactivity during sevoflurane anesthesia in healthy patients. Korean J Anesth 2020; 73(4): 311-8. doi: 10.4097/kja.19246. |
| 21. |
Rozet I, Metzner J, Brown M, et al. Dexmedetomidine does not affect evoked potentials during spine surgery. Anesth Analg 2015; 121(2): 492-501. doi: 10.1213/ANE.0000000000000840.
pmid: 26097987 |
| 22. | Janatmakan F, Nesioonpour S, Zadeh FJ, et al. Comparing the effect of clonidine and dexmedetomidine on intraoperative bleeding in spine surgery. Anesth Pain Med 2019; 9(1): e83967. doi: 10.5812/aapm.83967. |
| 23. |
Srivastava VK, Mishra A, Agrawal S, et al. Comparative evaluation of dexmedetomidine and magnesium sulphate on propofol consumption, haemodynamics and postoperative recovery in spine surgery: A prospective, randomized, placebo controlled, double-blind study. Adv Pharm Bull 2016; 6(1): 75-81. doi: 10.15171/apb.2016.012.
pmid: 27123421 |
| 24. | Yang L, Xu JM, Jiang X, et al. Effect of dexmedetomidine on plasma brain-derived neurotrophic factor: A double-blind, randomized and placebo-controlled study. Ups J Med Sci 2013; 118(4): 235-9. doi: 10.3109/03009734.2013.808295. |
| 25. | Ray M, Dalai CK, Ahmed SN, et al. A triple blind, randomised, placebo controlled, add-on trial to assess the efficacy and safety of dexmedetomidine in facilitation of general anaesthesia in patients undergoing elective spine surgery. Asian J Med Sci 2021; 12(3): 20-7. doi: https://doi.org/10.3126/ajms.v12i3.32831. |
| 26. |
Kim MH, Lee KY, Bae SJ, et al. Intraoperative dexmedetomidine attenuates stress responses in patients undergoing major spine surgery. Minerva Anestesiol 2019; 85(5): 468-77. doi: 10.23736/S0375-9393.18.12992-0.
pmid: 30226342 |
| 27. |
Kundra S, Taneja S, Choudhary A, et al. Effect of a low-dose dexmedetomidine infusion on intraoperative hemodynamics, anesthetic requirements and recovery profile in patients undergoing lumbar spine surgery. J Anaesthesiol Clin Pharmacol 2019; 35(2): 248-53. doi: 10.4103/joacp.JOACP_338_18.
pmid: 31303717 |
| 28. | Moharram AA, Mostafa RH. Efficacy of dexmedetomidine infusion without loading dose as a potent hypotensive agent in lumbar fixation surgery. Open Anesthesiol J 2019; 13(1): 68-74. doi: 10.2174/2589645801913010068. |
| 29. |
Nikoubakht N, Alimian M, Faiz S, et al. Effects of ketamine versus dexmedetomidine maintenance infusion in posterior spinal fusion surgery on acute postoperative pain. Surg Neurol Int 2021; 12: 192. doi: 10.25259/SNI_850_2020.
pmid: 34084620 |
| 30. | Liu T, Qin Y, Qi H, et al. A loading dose of dexmedetomidine with constant infusion inhibits intraoperative neuromonitoring during thoracic spinal decompression surgery: a randomized prospective study. Front Pharmacol 2022; 13: 840320. doi: 10.3389/fphar.2022.840320. |
| 31. |
Ebert TJ, Hall JE, Barney JA, et al. The effects of increasing plasma concentrations of dexmedetomidine in humans. Anesthesiology 2000; 93(2): 382-94. doi: 10.1097/00000542-200008000-00016.
pmid: 10910487 |
| 32. |
Bloor BC, Ward DS, Belleville JP, et al. Effects of intravenous dexmedetomidine in humans. II. Hemodynamic changes. Anesthesiology 1992; 77(6): 1134-42. doi: 10.1097/00000542-199212000-00014.
pmid: 1361311 |
| 33. |
Talke P, Lobo E, Brown R. Systemically administered alpha2-agonist-induced peripheral vasoconstriction in humans. Anesthesiology 2003; 99(1): 65-70. doi: 10.1097/00000542-200307000-00014.
pmid: 12826844 |
| 34. | Venn M, Newman J, Grounds M. A phase II study to evaluate the efficacy of dexmedetomidine for sedation in the medical intensive care unit. Intensive Care Med 2003; 29(2): 201-7. doi: 10.1007/s00134-002-1579-9. |
| 35. | Dutta S, Lal R, Karol MD, et al. Influence of cardiac output on dexmedetomidine pharmacokinetics. J Pharm Sci 2000; 89(4): 519-27. doi: 10.1002/(SICI)1520-6017(200004)89:4<519::AID-JPS9>3.0.CO;2-U. |
| 36. |
Pereira JV, Sanjanwala RM, Mohammed MK, et al. Dexmedetomidine versus propofol sedation in reducing delirium among older adults in the ICU: A systematic review and meta-analysis. Eur J Anaesthesiol 2020; 37(2): 121-31. doi: 10.1097/EJA.0000000000001131.
pmid: 31860605 |
| 37. |
Zhang L, Chen C, Wang L, et al. Awakening from anesthesia using propofol or sevoflurane with epidural block in radical surgery for senile gastric cancer. Int J Clin Exp Med 2015; 8(10): 19412-7.
pmid: 26770584 |
| 38. | Sneyd JR, Absalom AR, Barends C, et al. Hypotension during propofol sedation for colonoscopy: a retrospective exploratory analysis and meta-analysis. Br J Anaesth 2022; 128(4): 610-22. doi: 10.1016/j.bja.2021.10.044. |
| 39. | Wesselink EM, Kappen TH, Torn HM, et al. Intraoperative hypotension and the risk of postoperative adverse outcomes: a systematic review. Br J Anaesth 2018; 121(4): 706-21. doi: 10.1016/j.bja.2018.04.036. |
| 40. |
Waisbrod G, Mannion AF, Fekete TF, et al. Surgical training in spine surgery: safety and patient-rated outcome. Eur Spine J 2019; 28(4): 807-16. doi: 10.1007/s00586-019-05883-9.
pmid: 30694391 |
| 41. | Hathi K, Bigney E, Richardson E, et al. Minimally invasive vs. open surgery for lumbar spinal stenosis in patients with diabetes - A Canadian Spine Outcomes and Research Network study. Global Spine J 2023; 13(6): 1602-11. doi: 10.1177/21925682211042576. |
| 42. |
Chanbour H, Chen JW, Roth SG, et al. How much blood loss is too much for a 1-level open lumbar fusion. Int J Spine Surg 2023; 17(1): 146-55. doi: 10.14444/8395.
pmid: 36754572 |
| [1] | 田丽娟, 姚允泰, 袁素, 戴峥. 右美托咪定对老年患者围术期血流动力学稳定性影响的系统评价与Meta分析[J]. Chinese Medical Sciences Journal, 2023, 38(1): 1-10. |
| [2] | 白冰, 田园, 张越伦, 马满娇, 虞雪融, 黄宇光. 后路脊柱手术隐性失血的预测[J]. Chinese Medical Sciences Journal, 2019, 34(1): 38-44. |
| 阅读次数 | ||||||
|
全文 |
|
|||||
|
摘要 |
|
|||||
|