Chinese Medical Sciences Journal ›› 2022, Vol. 37 ›› Issue (2): 127-133.doi: 10.24920/003902
• Original Article • Previous Articles Next Articles
Phacoemulsification, Intraocular Lens Implantation, Goniosynechialysis, and Pseudo-Pupilloplasty for Refractory Acute Primary Angle Closure with Atonic Dilated Pupil
Erqian Wang, Ailing Bian, Yang Zhang, Shunhua Zhang*( )
)
- Department of Ophthalmology, Peking Union Medical College Hospital, Chinese Academy of Medical Sciences & Peking Union Medical College, Beijing 100730, China
-
Received:2021-03-23Accepted:2022-03-10Published:2022-06-30Online:2022-04-28 -
Contact:Shunhua Zhang E-mail:zhangshh@pumch.cn
Cite this article
Erqian Wang, Ailing Bian, Yang Zhang, Shunhua Zhang. Phacoemulsification, Intraocular Lens Implantation, Goniosynechialysis, and Pseudo-Pupilloplasty for Refractory Acute Primary Angle Closure with Atonic Dilated Pupil[J].Chinese Medical Sciences Journal, 2022, 37(2): 127-133.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
Table 1.
Preoperative characteristics of all the included patients"
| Patient’s no. | Gender | Age (yrs) | Attack duration (d) | BCVA (logMAR) | IOP (mmHg) | ACD (mm) | Pupil diameter (mm) | CECC (cells/mm2) | AL (mm) |
|---|---|---|---|---|---|---|---|---|---|
| 1 | F | 77 | 3 | 1.31 | 38 | 1.87 | 6.0 | 2415 | 22.55 |
| 2 | F | 73 | 5 | 1.52 | 54 | 1.90 | 6.5 | - | 21.85 |
| 3 | F | 62 | 7 | 1.10 | 45 | 1.67 | 6.0 | 2350 | 21.38 |
| 4 | F | 80 | 10 | 1.00 | 35 | 2.05 | 5.5 | 1980 | 21.35 |
| 4 | F | 80 | 2 | 0.70 | 38 | 1.95 | 5.5 | 1766 | 21.18 |
| 5 | F | 78 | 20 | 2.00 | 48 | 1.80 | 5.5 | - | 20.92 |
| 6 | M | 74 | 7 | 1.00 | 38 | 1.96 | 6.0 | 2100 | 21.83 |
| 7 | M | 67 | 10 | 2.00 | 49 | 1.89 | 5.5 | 1655 | 22.08 |
| 8 | F | 67 | 10 | 2.00 | 41 | 1.66 | 5.5 | - | 21.15 |
| 9 | M | 67 | 11 | 2.00 | 60 | 1.75 | 5.5 | 1890 | 22.40 |
| 10 | F | 71 | 5 | 1.00 | 36 | 1.95 | 5.5 | 2100 | 21.62 |
| 11 | M | 72 | 5 | 0.92 | 45 | 1.90 | 5.5 | - | 22.82 |
| 12 | F | 71 | 16 | 0.52 | 48 | 1.11 | 5.0 | 2153 | 21.06 |
| 13 | F | 63 | 25 | 1.00 | 40 | 1.72 | 5.5 | - | 22.86 |
| 14 | F | 64 | 22 | 0.60 | 48 | 1.65 | 5.0 | 2966 | 21.61 |
| 15 | F | 66 | 13 | 2.00 | 52 | 1.68 | 5.5 | - | 21.68 |
| 16 | F | 76 | 18 | 1.00 | 35 | 1.82 | 6.0 | 2726 | 22.43 |
| 17 | F | 47 | 28 | 0.70 | 66 | 1.76 | 6.5 | 1760 | 21.81 |
| 18 | F | 77 | 26 | 0.30 | 22 | 1.57 | 5.0 | 2252 | 22.21 |
| 19 | F | 77 | 10 | 0.92 | 42 | 1.75 | 5.0 | 1874 | 21.79 |
| Mean±SD | 70.5±7.9 | 12.7±8.0 | 1.18±0.55 | 44.0±9.8 | 1.77±0.21 | 5.6±0.4 | NA | 21.81±0.62 |
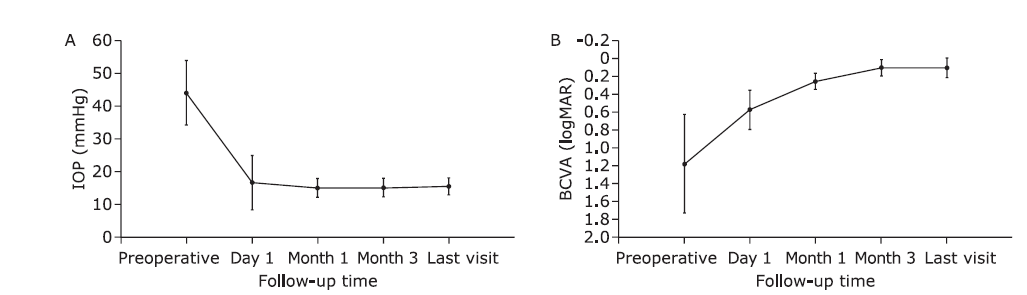
Table 2.
Preoperative and postoperative comparisons of BCVA, IOP, and ACD"
| Patient’s no. | BCVA (logMAR) | IOP (mmHg) | ACD (mm) | Residual PAS (degree) | Number of medications | |||||
|---|---|---|---|---|---|---|---|---|---|---|
| Pre | Post* | Pre | Post* | Pre | Post* | |||||
| 1 | 1.31 | 0.00 | 38 | 14 | 1.87 | 3.49 | 90 | 0 | ||
| 2 | 1.52 | 0.10 | 54 | 12 | 1.90 | 3.23 | 0 | 0 | ||
| 3 | 1.10 | 0.10 | 45 | 14 | 1.67 | 3.05 | 150 | 0 | ||
| 4 | 1.00 | 0.22 | 35 | 15 | 2.05 | 3.56 | 0 | 0 | ||
| 4 | 0.70 | 0.30 | 38 | 16 | 1.95 | 3.42 | 0 | 0 | ||
| 5 | 2.00 | 0.00 | 48 | 19 | 1.80 | 3.23 | 180 | 3 | ||
| 6 | 1.00 | 0.22 | 38 | 20 | 1.96 | 3.35 | 90 | 1 | ||
| 7 | 2.00 | 0.10 | 49 | 16 | 1.89 | 3.52 | 0 | 0 | ||
| 8 | 2.00 | 0.22 | 41 | 15 | 1.66 | 3.11 | 90 | 0 | ||
| 9 | 2.00 | -0.08 | 60 | 17 | 1.75 | 3.48 | 0 | 0 | ||
| 10 | 1.00 | 0.10 | 36 | 16 | 1.95 | 3.42 | 0 | 0 | ||
| 11 | 0.92 | 0.00 | 45 | 17 | 1.90 | 3.74 | 60 | 0 | ||
| 12 | 0.52 | 0.10 | 48 | 14 | 1.11 | 3.57 | 10 | 0 | ||
| 13 | 1.00 | 0.00 | 40 | 20 | 1.72 | 3.34 | 240 | 1 | ||
| 14 | 0.60 | 0.22 | 48 | 14 | 1.65 | 3.38 | 120 | 0 | ||
| 15 | 2.00 | 0.22 | 52 | 10 | 1.68 | 3.29 | 90 | 0 | ||
| 16 | 1.00 | 0.00 | 35 | 14 | 1.82 | 3.66 | 60 | 0 | ||
| 17 | 0.70 | 0.10 | 66 | 16 | 1.76 | 3.31 | 60 | 0 | ||
| 18 | 0.30 | 0.00 | 22 | 17 | 1.57 | 3.62 | 0 | 0 | ||
| 19 | 0.92 | 0.30 | 42 | 17 | 1.75 | 3.40 | 0 | 0 | ||
| Mean±SD | 1.18±0.55 | 0.11±0.11 | 44.0±9.8 | 15.5±2.6 | 1.77±0.21 | 3.40±0.20 | 69±73 | 0.29±0.77 | ||

Figure 2.
The preoperative and postoperative changes of anterior capsule residue and gradual formation of pseudo-pupil in a 77-year-old female. A. Anterior segment photograph before surgery. B-F. Anterior segment photography at postoperative day 1, month 1, month 3, year 2, and year 3. Note that an oval hole or the pseudo-pupil was completely formed based on the anterior capsule residue at postoperative month 3 (D)."
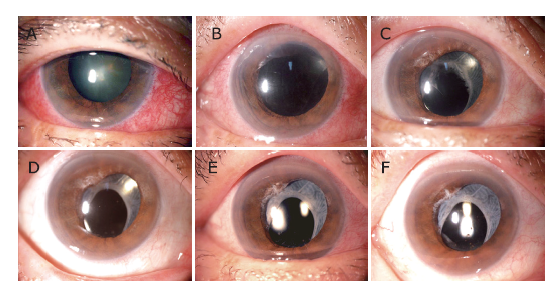

Figure 3.
Color fundus photograph of the same eye illustrated in Figure 2 taken at postoperative year 2 with Topcon TRC-50DX Fundus Camera (Topcon Corp., Tokyo, Japan). The visualization of posterior pole and midperipheral retina is satisfactory, although the areas at or anterior to equator is obscure, dim, or even invisible."

| 1. |
Lam DS, Leung DY, Tham CC, et al. Randomized trial of early phacoemulsification versus peripheral iridotomy to prevent intraocular pressure rise after acute primary angle closure. Ophthalmology 2008; 115(7):1134-40. doi: 10.1016/j.ophtha.2007.10.033.
doi: 10.1016/j.ophtha.2007.10.033 |
| 2. |
Gupta S, Sethi A, Yadav S, et al. Safety and efficacy of incisional goniotomy as an adjunct with phacoemulsification in primary angle-closure glaucoma. J Cataract Refract Surg 2021; 47(4):504-11. doi: 10.1097/j.jcrs.0000000000000481.
doi: 10.1097/j.jcrs.0000000000000481 |
| 3. |
Teekhasaenee C, Ritch R. Combined phacoemulsification and goniosynechialysis for uncontrolled chronic angle-closure glaucoma after acute angle-closure glaucoma. Ophthalmology 1999; 106(4):669-74. doi: 10.1016/S0161-6420(99)90149-5.
doi: 10.1016/S0161-6420(99)90149-5 pmid: 10201585 |
| 4. |
Zuo C, Long B, Guo X, et al. Effect of phacoemulsification on anterior chamber angle in eyes with medically uncontrolled filtered primary angle-closure glaucoma. J Ophthalmol 2020; 2020:8720450. doi: 10.1155/2020/8720450.
doi: 10.1155/2020/8720450 |
| 5. |
Harasymowycz PJ, Papamatheakis DG, Ahmed I, et al. Phacoemulsification and goniosynechialysis in the management of unresponsive primary angle closure. J Glaucoma 2005; 14(3):186-9. doi: 10.1097/01.ijg.0000159131.38828.85.
doi: 10.1097/01.ijg.0000159131.38828.85 pmid: 15870598 |
| 6. |
Elwehidy AS, Bayoumi NHL, Badawi AE, et al. Combined phacoemulsification-viscosynechialysis-trabeculotomy vs phacotrabeculectomy in uncontrolled primary angle-closure glaucoma with cataract. J Cataract Refract Surg 2019; 45(12):1738-45. doi: 10.1016/j.jcrs.2019.07.031.
doi: 10.1016/j.jcrs.2019.07.031 |
| 7. |
Lin YH, Wu CH, Huang SM, et al. Early versus delayed phacoemulsification and intraocular lens implantation for acute primary angle-closure. J Ophthalmol 2020; 2020:8319570. doi: 10.1155/2020/8319570.
doi: 10.1155/2020/8319570 |
| 8. |
Tian T, Li M, Pan Y, et al. The effect of phacoemulsification plus goniosynechialysis in acute and chronic angle closure patients with extensive goniosynechiae. BMC Ophthalmol 2019; 19(1):65. doi: 10.1186/s12886-019-1070-9.
doi: 10.1186/s12886-019-1070-9 pmid: 30832600 |
| 9. |
Tan GS, Hoh ST, Husain R, et al. Visual acuity after acute primary angle closure and considerations for primary lens extraction. Br J Ophthalmol 2006; 90(1):14-6. doi: 10.1136/bjo.2005.077115.
doi: 10.1136/bjo.2005.077115 |
| 10. |
Maeda M, Watanabe M, Ichikawa K. Goniosynechialysis using an ophthalmic endoscope and cataract surgery for primary angle-closure glaucoma. J Glaucoma 2014; 23(3):174-8. doi: 10.1097/IJG.0b013e31826aaf3b.
doi: 10.1097/IJG.0b013e31826aaf3b |
| 11. |
Espana EM, Ioannidis A, Tello C, et al. Urrets-Zavalia syndrome as a complication of argon laser peripheral iridoplasty. Br J Ophthalmol 2007; 91(4):427-9. doi: 10.1136/bjo.2006.105098.
doi: 10.1136/bjo.2006.105098 |
| 12. |
Wang Y, Zhao K, Jin Y, et al. Changes of higher order aberration with various pupil sizes in the myopic eye. J Refract Surg 2003; 19(2 Suppl):S270-4. doi: 10.3928/1081-597X-20030302-21.
doi: 10.3928/1081-597X-20030302-21 pmid: 12699188 |
| 13. |
Hansapinyo L, Choy BNK, Lai JSM, et al. Phacoemulsification versus phacotrabeculectomy in primary angle-closure glaucoma with cataract: long-term clinical outcomes. J Glaucoma 2020; 29(1):15-23. doi: 10.1097/IJG.0000000000001397.
doi: 10.1097/IJG.0000000000001397 pmid: 31702714 |
| 14. |
Jacobi PC, Dietlein TS, Luke C, et al. Primary phacoemulsification and intraocular lens implantation for acute angle-closure glaucoma. Ophthalmology 2002; 109(9):1597-603. doi: 10.1016/s0161-6420(02)01123-5.
doi: 10.1016/s0161-6420(02)01123-5 |
| 15. |
Narang P, Agarwal A, Kumar DA. Single-pass four-throw pupilloplasty for angle-closure glaucoma. Indian J Ophthalmol 2018; 66(1):120-4. doi: 10.4103/ijo.IJO_559_17.
doi: 10.4103/ijo.IJO_559_17 pmid: 29283136 |
| No related articles found! |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||
|