Chinese Medical Sciences Journal ›› 2023, Vol. 38 ›› Issue (3): 206-217.doi: 10.24920/004198
中药复方防感汤对SARS-CoV-2刺突蛋白引起的肺和结肠上皮细胞损伤的保护作用与TGF-β/Smad2/3和NF-κB通路的调节有关
- 深圳大学第二附属医院(深圳市宝安区人民医院)中医科,深圳518100,广东省,中国
-
收稿日期:2022-12-06接受日期:2023-06-05出版日期:2023-09-30发布日期:2023-07-04 -
通讯作者:* 沈维增, E-mail:shenweizeng@163.com 。
A Chinese Herb Prescription “Fang-gan Decoction” Protects Against Damage to Lung and Colon Epithelial Cells Caused by the SARS-CoV-2 Spike Protein by Regulating the TGF-β/Smad2/3 and NF-κB Pathways
Chao Huang,Hao-Sheng Liu,Bing-Jun Liang,Sheng-Rong Liao,Wei-Zeng Shen*( )
)
- Department of Traditional Chinese Medicine, the Second Affiliated Hospital of Shenzhen University (People’s Hospital of Shenzhen Baoan District), Shenzhen 518101, Guangdong Province, China
-
Received:2022-12-06Accepted:2023-06-05Published:2023-09-30Online:2023-07-04 -
Contact:* E-mail:shenweizeng@163.com .
摘要:
背景与目的 探讨中药复方防感汤对SARS-CoV-2刺突蛋白诱导的肺、肠损伤的体外和体内保护作用及其机制。
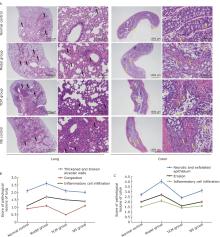
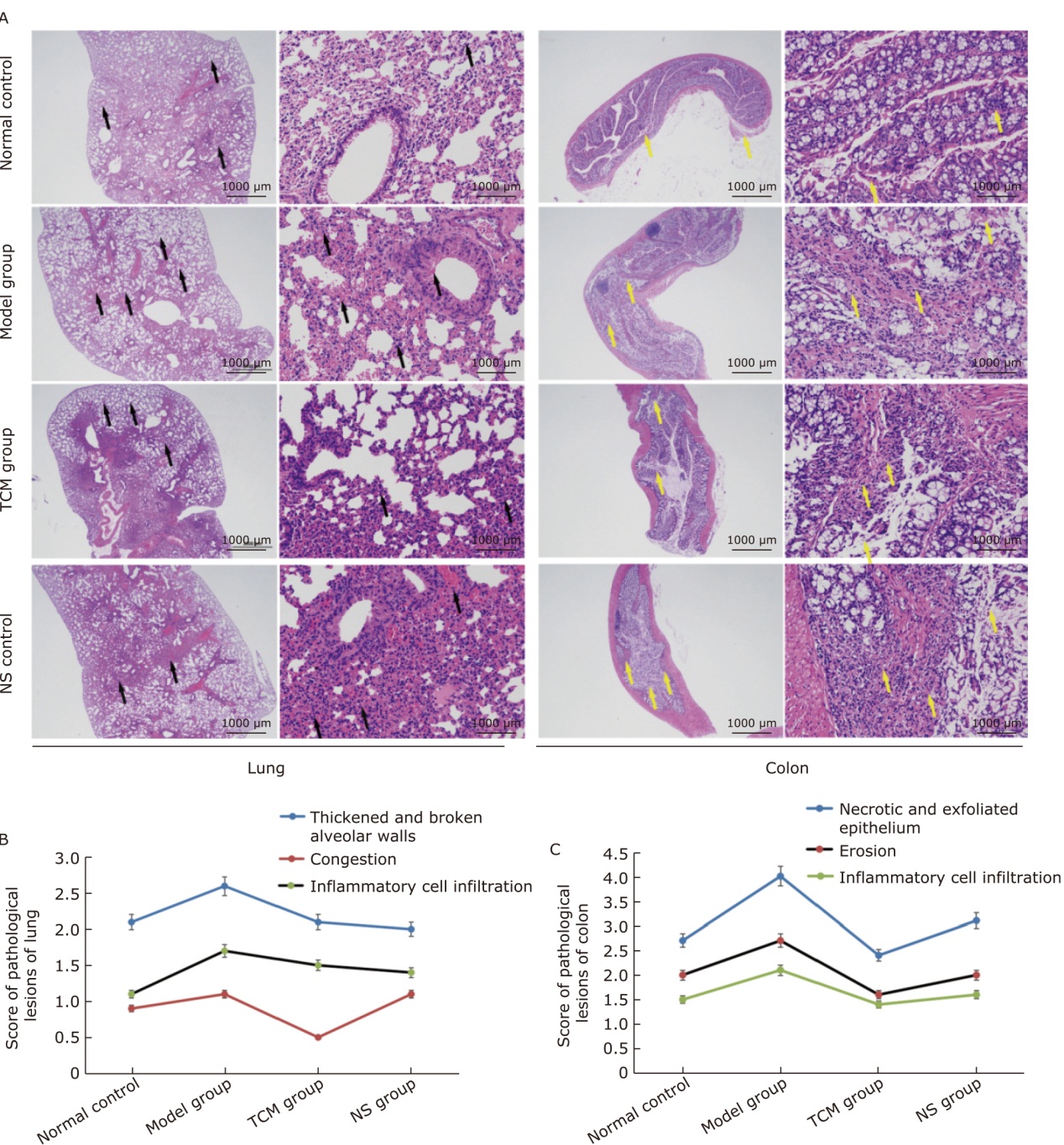
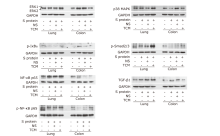
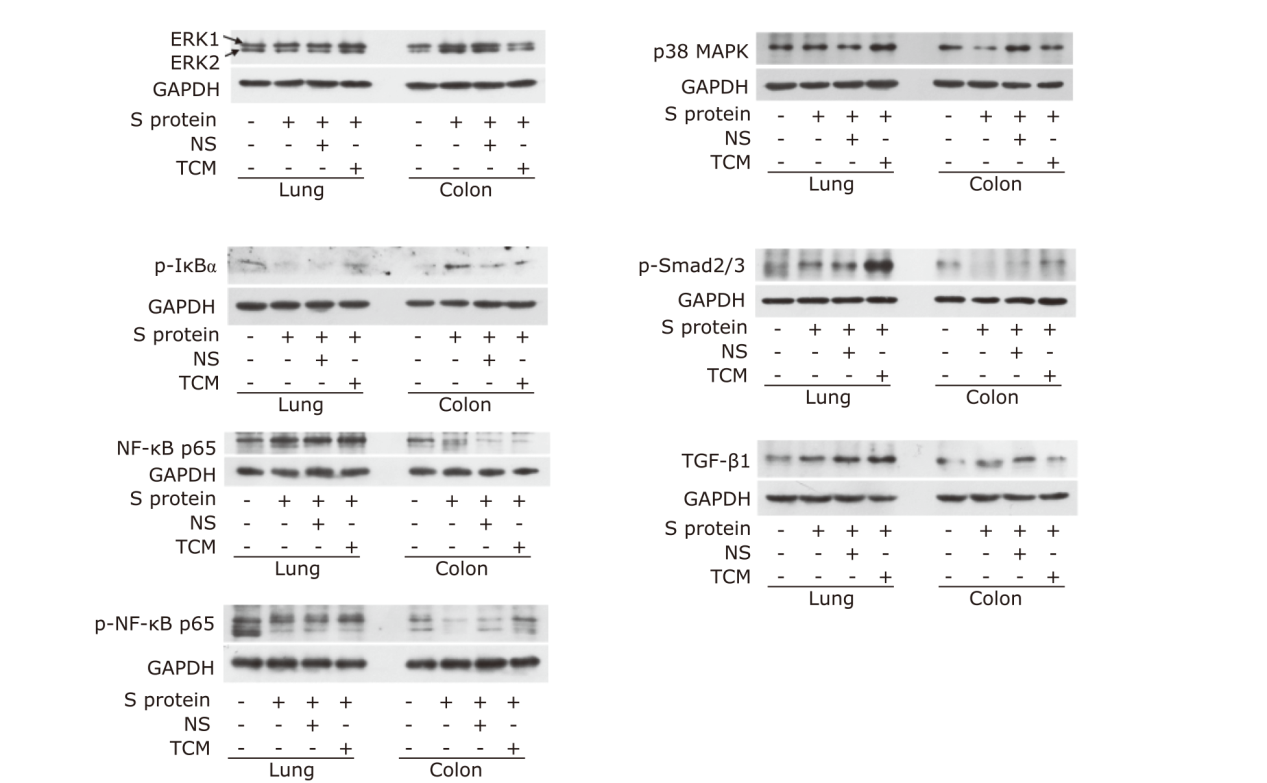
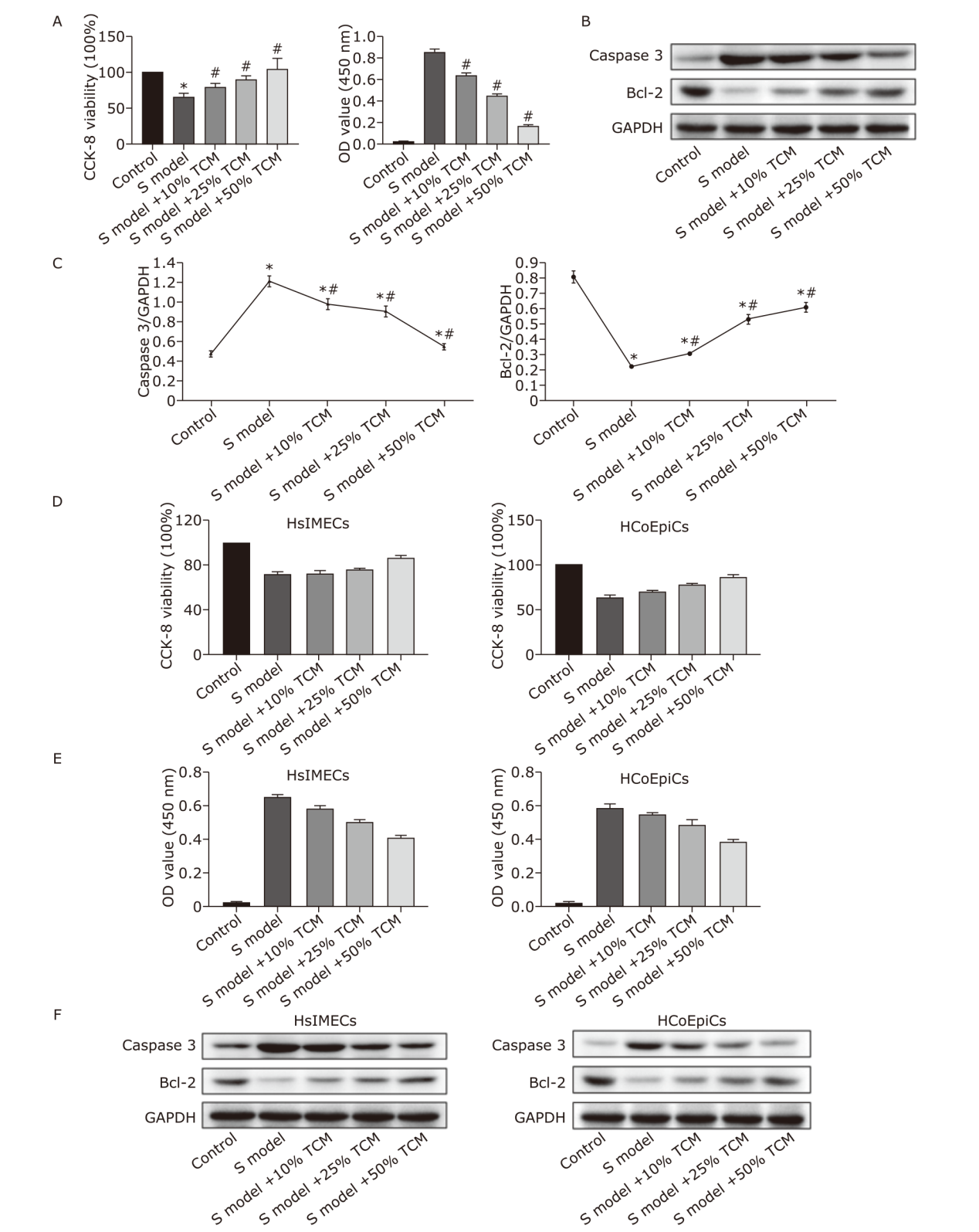
方法 用重组SARS-CoV-2刺突蛋白刺激BALB/c雌性小鼠和3株经防感汤预处理的细胞系。检测各组组织苏木精-伊红(HE)染色、病理评分、细胞通透性和活力以及肺、结肠ACE2表达。酶联免疫吸附测定法(ELISA)检测小鼠血清和细胞上清中炎症因子水平。蛋白质印迹法(Western blotting)检测NF-κB p65、p-NF-κB p65、p- IκB α、p-Smad2/3、TGF-β1、Caspase3、Bcl-2的表达。
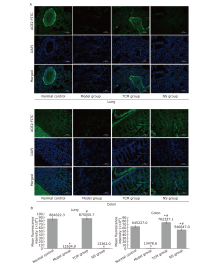
结果 从病理评分以及细胞通透性和活力来看,中草药在体内和体外均对刺突蛋白诱发的肺和结肠损伤均有保护作用(P<0.05)。中草药上调肺和结肠中被刺突蛋白降低的ACE2表达,显著改善刺突蛋白引起的炎症标志物的分泌紊乱,同时调节TGF-β/Smads和NF-κB通路的活性。
结论 中药复方防感汤对SARS-CoV-2刺突蛋白刺激的肺和肠组织损伤具有一定的保护作用,其机制基于对可能具有组织类型特异的NF-κB和TGF-β1/Smad通路的调控作用。
引用本文
Chao Huang, Hao-Sheng Liu, Bing-Jun Liang, Sheng-Rong Liao, Wei-Zeng Shen. A Chinese Herb Prescription “Fang-gan Decoction” Protects Against Damage to Lung and Colon Epithelial Cells Caused by the SARS-CoV-2 Spike Protein by Regulating the TGF-β/Smad2/3 and NF-κB Pathways[J].Chinese Medical Sciences Journal, 2023, 38(3): 206-217.
"
| Markers | Time | Normal group | Model Gorup | NS group | TCM group | P value |
|---|---|---|---|---|---|---|
| IL-6 | 3d | 644.61 | 717.36* | 696.89* | 702.85* | 0.009 |
| 5d | 268.02 | 342.09* | 344.88* | 298.89#? | <0.001 | |
| IL-10 | 3d | 25.14 | 82.12* | 74.86* | 44.7# | 0.009 |
| 5d | 87.61 | 145.79* | 123.84* | 121.52 | 0.019 | |
| IL-13 | 3d | 352.69 | 344.69 | 362.46 | 351.09 | 0.998 |
| 5d | 91.9 | 102.87 | 92.42 | 100.23 | 0.931 | |
| TNF-α | 3d | 566.19 | 853.87 | 840.04 | 633.38 | 0.141 |
| 5d | 575.77 | 1042.36* | 1236.73*# | 864.43*#? | <0.001 | |
| CRP | 3d | 18175.8 | 21129.27* | 21550.72* | 19786.15 | 0.042 |
| 5d | 5933.09 | 7413.08* | 6567.13# | 6093.33# | 0.001 |
"
| Markers | Control group | S model group | S model+10% TCM group | S model+25% TCM group | S model+50% TCM group | P value |
|---|---|---|---|---|---|---|
| IL-6 (ng/L) | 20.24 | 33.01* | 29.81*# | 27.95*# | 20.01# | <0.001 |
| IL-10 (ng/L) | 428.32 | 435.40 | 435.54 | 435.38 | 418.36 | 0.762 |
| IL-13 (ng/L) | 41.33 | 27.17* | 30.75*# | 33.67*# | 35.04*# | <0.001 |
| TNF-α (ng/L) | 212.14 | 309.29* | 277.51* | 263.84 | 222.83 | <0.001 |
| NF-κB (ng/L) | 215.69 | 187.85 | 183.57 | 206.98 | 213.29 | 0.154 |
| TGF-β1 (ng/L) | 285.49 | 156.97* | 185.03*# | 196.94*# | 272.26# | <0.001 |
"
| Cells | Markers | Control group | S model group | S model+10% TCM group | S model+25% TCM group | S model+50% TCM group | P value |
|---|---|---|---|---|---|---|---|
| HsIMECs | IL-6 (ng/L) | 22.40 | 30.49* | 27.62* | 25.39# | 22.11# | <0.001 |
| IL-10 (ng/L) | 348.14 | 307.22* | 318.12* | 327.84*# | 339.72# | 0.001 | |
| IL-13 (ng/L) | 30.47 | 30.59 | 28.49 | 31.09 | 29.16 | 0.757 | |
| TNF-α (ng/L) | 121.90 | 273.29* | 271.30* | 234.02* | 202.70*# | <0.001 | |
| NF-κB (ng/L) | 178.52 | 177.08 | 175.88 | 178.74 | 180.86 | 0.859 | |
| TGF-β1 (ng/L) | 149.71 | 146.78 | 143.00 | 141.65 | 145.37 | 0.986 | |
| HCoEpiCs | IL-6 (ng/L) | 24.13 | 28.28* | 25.26# | 23.78# | 21.95# | 0.001 |
| IL-10 (ng/L) | 372.10 | 384.02 | 378.86 | 388.56 | 388.92 | 0.910 | |
| IL-13 (ng/L) | 23.69 | 15.99* | 20.01 | 22.77# | 21.53# | 0.021 | |
| TNF-α (ng/L) | 168.63 | 286.16* | 281.62* | 230.50*# | 221.83*# | <0.001 | |
| NF-κB (ng/L) | 133.02 | 131.88 | 134.09 | 126.03 | 134.28 | 0.201 | |
| TGF-β1 (ng/L) | 177.31 | 173.80 | 176.35 | 177.77 | 171.37 | 0.452 |
| 1 | Wang C, Horby PW, Hayden FG, et al. A novel coronavirus outbreak of global health concern. The Lancet 2020; 395(10223): 470-3. doi: 10.1016/S0140-6736(20)30185-9. |
| 2 | Ozturkler Z, Kalkan R. A new perspective of COVID-19 infection: An epigenetics point of view. Glob Med Genet 2021; 9(1): 4-6. doi: 10.1055/s-0041-1736565. |
| 3 |
Girma D, Dejene H, Adugna L, et al. COVID-19 case fatality rate and factors contributing to mortality in Ethiopia: A systematic review of current evidence. Infect Drug Resist, 2022, 15: 3491-501. doi: 10.2147/IDR.S369266.
pmid: 35813083 |
| 4 | Huang K, Zhang P, Zhang Z, et al. Traditional Chinese Medicine (TCM) in the treatment of COVID-19 and other viral infections: Efficacies and mechanisms. Pharmacol Ther 2021; 225: 107843. doi: 10.1016/j.pharmthera.2021.107843. |
| 5 | Zhao Z, Li Y, Zhou L, et al. Prevention and treatment of COVID-19 using Traditional Chinese Medicine: A review. Phytomedicine 2021; 85: 153308. doi: 10.1016/j.phymed.2020.153308. |
| 6 |
Feng Z, Yang J, Xu M, et al. Dietary supplements and herbal medicine for COVID-19: A systematic review of randomized control trials. Clin Nutr ESPEN 2021; 44: 50-60. doi: 10.1016/j.clnesp.2021.05.018.
pmid: 34330513 |
| 7 |
An X, Zhang Y, Duan L, et al. The direct evidence and mechanism of traditional Chinese medicine treatment of COVID-19. Biomed Pharmacother 2021; 137: 111267. doi: 10.1016/j.biopha.2021.111267.
pmid: 33508618 |
| 8 | Ren JL, Zhang AH, Wang XJ. Traditional Chinese medicine for COVID-19 treatment. Pharmacol Res 2020; 155: 104743. doi: 10.1016/j.phrs.2020.104743. |
| 9 | Wang Z, Yang L. Chinese herbal medicine: Fighting SARS-CoV-2 infection on all fronts. J Ethnopharmacol 2021; 270: 113869. doi: 10.1016/j.jep.2021.113869. |
| 10 | Ji Z, Hu H, Qiang X, et al. Traditional Chinese Medicine for COVID-19: A Network meta-analysis and systematic review. Am J Chin Med 2022; 50(4): 883-925. doi: 10.1142/S0192415X22500379. |
| 11 | Huang K, Zhang P, Zhang Z, et al. Traditional Chinese medicine (TCM) in the treatment of COVID-19 and other viral infections: Efficacies and mechanisms. Pharmacol Ther 2021; 225: 107843. doi: 10.1016/j.pharmthera.2021.107843. |
| 12 | Patel KP, Patel PA, Vunnam RR, et al. Gastrointestinal, hepatobiliary, and pancreatic manifestations of COVID-19. J Clin Virol 2020; 128: 104386. doi: 10.1016/j.jcv.2020.104386. |
| 13 | Galanopoulos M, Gkeros F, Doukatas A, et al. COVID-19 pandemic: Pathophysiology and manifestations from the gastrointestinal tract. World J Gastroenterol 2020; 26(31): 4579-88. doi: 10.3748/wjg.v26.i31.4579. |
| 14 |
Jin X, Lian JS, Hu JH, et al. Epidemiological, clinical and virological characteristics of 74 cases of coronavirus-infected disease 2019 (COVID-19) with gastrointestinal symptoms. Gut 2020; 69(6): 1002-9. doi: 10.1136/gutjnl-2020-320926.
pmid: 32213556 |
| 15 |
Hunt RH, East JE, Lanas A, et al. COVID-19 and gastrointestinal disease: Implications for the gastroenterologist. Dig Dis 2021; 39(2): 119-39. doi: 10.1159/000512152.
pmid: 33040064 |
| 16 |
Bojkova D, Wagner JUG, Shumliakivska M, et al. SARS-CoV-2 infects and induces cytotoxic effects in human cardiomyocytes. Cardiovasc Res 2020; 116(14): 2207-15. doi: 10.1093/cvr/cvaa267.
pmid: 32966582 |
| 17 |
Corpetti C, Del Re A, Seguella L, et al. Cannabidiol inhibits SARS-Cov-2 spike (S) protein-induced cytotoxicity and inflammation through a PPARγ-dependent TLR4/NLRP3/Caspase-1 signaling suppression in Caco-2 cell line. Phytother Res 2021; 35(12): 6893-903. doi: 10.1002/ptr.7302.
pmid: 34643000 |
| 18 |
Mannar D, Saville JW, Zhu X, et al. SARS-CoV-2 Omicron variant: Antibody evasion and cryo-EM structure of spike protein-ACE2 complex. Science 2022; 375(6582): 760-4. doi: 10.1126/science.abn7760.
pmid: 35050643 |
| 19 |
Ashraf UM, Abokor AA, Edwards JM, et al. SARS-CoV-2, ACE 2 expression, and systemic organ invasion. Physiol Genomics 2021; 53(2): 51-60. doi: 10.1152/physiolgenomics.00087.2020.
pmid: 33275540 |
| 20 |
Lv Y, Wang S, Liang P, et al. Screening and evaluation of anti-SARS-CoV-2 components from Ephedra sinica by ACE2/CMC-HPLC-IT-TOF-MS approach. Anal Bioanal Chem 2021; 413(11): 2995-3004. doi: 10.1007/s00216-021-03233-7.
pmid: 33608752 |
| 21 | Babapoor-Farrokhran S, Gill D, Walker J, et al. Myocardial injury and COVID-19: Possible mechanisms. Life Sci 2020; 253: 117723. doi: 10.1016/j.lfs.2020.117723. |
| 22 | Colunga Biancatelli RML, Solopov PA, Sharlow ER, et al. The SARS-CoV-2 spike protein subunit S1 induces COVID-19-like acute lung injury in Κ18-hACE2 transgenic mice and barrier dysfunction in human endothelial cells. Am J Physiol Lung Cell Mol Physiol 2021; 321(2): L477-84. doi: 10.1152/ajplung.00223.2021. |
| 23 |
Hekman RM, Hume AJ, Goel RK, et al. Actionable cytopathogenic host responses of human alveolar type 2 cells to SARS-CoV-2. Mol Cell 2020; 80(6): 1104-22.e9. doi: 10.1016/j.molcel.2020.11.028.
pmid: 33259812 |
| 24 |
Chen J, Wang W, Tang Y, et al. Inflammatory stress in SARS-COV-2 associated acute kidney injury. Int J Biol Sci 2021; 17(6): 1497-506. doi: 10.7150/ijbs.58791.
pmid: 33907513 |
| 25 | Wang W, Chen J, Hu D, et al. SARS-CoV-2 N protein induces acute kidney injury via Smad3-dependent G 1 cell cycle arrest mechanism. Adv Sci (Weinh) 2022; 9(3): e2103248. doi: 10.1002/advs.202103248. |
| 26 |
Vaz de Paula CB, Nagashima S, et al. IL-4/IL-13 remodeling pathway of COVID-19 lung injury. Sci Rep 2020; 10(1): 18689. doi: 10.1038/s41598-020-75659-5.
pmid: 33122784 |
| 27 | Lu Y, Zhang Y, Pan Z, et al. Potential “therapeutic” effects of tocotrienol-rich fraction (TRF) and carotene “against” bleomycin-induced pulmonary fibrosis in rats via TGF-β/Smad, PI3K/Akt/mTOR and NF-κB signaling pathways. Nutrients 2022; 14(5): 1094. doi: 10.3390/nu14051094. |
| 28 | Wang W, Chen J, Hu D, et al. SARS-CoV-2 N protein induces acute kidney injury via Smad3-dependent G 1 cell cycle arrest mechanism. Adv Sci (Weinh) 2022; 9(3): e2103248. doi: 10.1002/advs.202103248. |
| 29 | Cui Y, Xin H, Tao Y, et al. Arenaria kansuensis attenuates pulmonary fibrosis in mice via the activation of Nrf2 pathway and the inhibition of NF-kB/TGF-beta1/Smad2/3 pathway. Phytother Res 2021; 35(2): 974-86. doi: 10.1002/ptr.6857. |
| 30 | Zheng M, Karki R, Williams EP, et al. TLR2 senses the SARS-CoV-2 envelope protein to produce inflammatory cytokines. Nat Immunol 2021; 22(7): 829-38. doi: 10.1038/s41590-021-00937-x. |
| 31 | Moustaqil M, Ollivier E, Chiu HP, et al. SARS-CoV-2 proteases PLpro and 3CLpro cleave IRF3 and critical modulators of inflammatory pathways (NLRP12 and TAB1): implications for disease presentation across species. Emerg Microbes Infect 2021 10(1): 178-95. doi: 10.1080/22221751.2020.1870414. |
| 32 |
Tan Y, Tang F. SARS-CoV-2-mediated immune system activation and potential application in immunotherapy. Med Res Rev 2021; 41(2): 1167-94. doi: 10.1002/med.21756.
pmid: 33185926 |
| 33 | Petruk G, Puthia M, Petrlova J, et al. SARS-CoV-2 spike protein binds to bacterial lipopolysaccharide and boosts proinflammatory activity. J Mol Cell Biol 2020; 12(12): 916-32. doi: 10.1093/jmcb/mjaa067. |
| 34 | Karwaciak I, Karaś K, Sałkowska A, et al. Chlorpromazine, a clinically approved drug, inhibits SARS-CoV-2 nucleocapsid-mediated induction of IL-6 in human monocytes. Molecules 2022; 27(12): 3651. doi: 10.3390/molecules27123651. |
| 35 |
Sharma VK, Prateeksha, Singh SP, et al. Nanocurcumin potently inhibits SARS-CoV-2 Spike protein-induced cytokine storm by deactivation of MAPK/NF-κB signaling in epithelial cells. ACS Appl Bio Mater 2022; 5(2): 483-91. doi: 10.1021/acsabm.1c00874.
pmid: 35112841 |
| 36 | DuShane JK, Wilczek MP, Mayberry CL, et al. ERK is a critical regulator of JC polyomavirus infection. J Virol 2018; 92(7)): e01529-17. doi: 10.1128/JVI.01529-17. |
| 37 |
Ghasemnejad-Berenji M, Pashapour S. SARS-CoV-2 and the possible role of Raf/MEK/ERK pathway in viral survival: is this a potential therapeutic strategy for COVID-19? Pharmacology 2021; 106(1-2): 119-22. doi: 10.1159/000511280.
pmid: 33011728 |
| 38 |
Schreiber A, Viemann D, Schöning J, et al. The MEK1/2-inhibitor ATR-002 efficiently blocks SARS-CoV-2 propagation and alleviates pro-inflammatory cytokine/chemokine responses. Cell Mol Life Sci 2022; 79(1): 65. doi: 10.1007/s00018-021-04085-1.
pmid: 35013790 |
| 39 | Zeng FM, Li YW, Deng ZH, et al. SARS-CoV-2 spike spurs intestinal inflammation via VEGF production in enterocytes. EMBO Mol Med 2022; 14(5): e14844. doi: 10.15252/emmm.202114844. |
| 40 | Xie P, Fang Y, Shen Z, et al. Broad antiviral and anti-inflammatory activity of Qingwenjiere mixture against SARS-CoV-2 and other human coronavirus infections. Phytomedicine 2021; 93: 153808. doi: 10.1016/j.phymed.2021.153808. |
| 41 |
Neufeldt CJ, Cerikan B, Cortese M, et al. SARS-CoV-2 infection induces a pro-inflammatory cytokine response through cGAS-STING and NF-κB. Commun Biol 2022; 5(1): 45. doi: 10.1038/s42003-021-02983-5.
pmid: 35022513 |
| 42 | Wu Y, Ma L, Cai S, et al. RNA-induced liquid phase separation of SARS-CoV-2 nucleocapsid protein facilitates NF-κB hyper-activation and inflammation. Signal Transduct Target Ther 2021; 6(1): 167. doi: 10.1038/s41392-021-00575-7. |
| 43 | Robles JP, Zamora M, Adan-Castro E, et al. The spike protein of SARS-CoV-2 induces endothelial inflammation through integrin α5β1 and NF-κB signaling. J Biol Chem 2022; 298(3): 101695. doi: 10.1016/j.jbc.2022.101695. |
| 44 | Colunga Biancatelli RML, Solopov PA, Sharlow ER, et al. The SARS-CoV-2 spike protein subunit S1 induces COVID-19-like acute lung injury in Κ18-hACE2 transgenic mice and barrier dysfunction in human endothelial cells. Am J Physiol Lung Cell Mol Physiol 2021; 321(2): L477-84. doi: 10.1152/ajplung.00223.2021. |
| 45 | Xia J, Tang W, Wang J, et al. SARS-CoV-2 N protein induces acute lung injury in mice via NF-ĸB activation. Front Immunol 2021; 12: 791753. doi: 10.3389/fimmu.2021.791753. |
| [1] | 陈晓勇, 蔡宏媛, 刘忆南, 洪晶. 短疗程睑缘清洁联合抗生素滴眼液的使用对白内障术前眼表菌群抑制作用的临床研究[J]. Chinese Medical Sciences Journal, 2022, 37(2): 118-126. |
| [2] | 王尔茜, 卞爱玲, 张扬, 张顺华. 超声乳化白内障摘除、人工晶状体植入、房角分离联合假瞳孔成形治疗伴有瞳孔散大固定的难治性急性闭角型青光眼[J]. Chinese Medical Sciences Journal, 2022, 37(2): 127-133. |
| [3] | 田毅, 龚亚红, 柳培雨, 王晟, 徐宵寒, 王晓月, 黄宇光. 新型冠状病毒肺炎流行期间围术期感染的防控策略[J]. Chinese Medical Sciences Journal, 2020, 35(2): 114-120. |
| 阅读次数 | ||||||
|
全文 |
|
|||||
|
摘要 |
|
|||||
|