Chinese Medical Sciences Journal ›› 2024, Vol. 39 ›› Issue (1): 29-45.doi: 10.24920/004281
Previous Articles Next Articles
Body Positions Alter Hemodynamics and Respiration in Healthy Adults: A Systematic Review and Meta-Analysis
Ruchada Sriamad, Sirinut Chaiduang, Thaniya Klinsophon, Premtip Thaveeratitham*( )
)
- Department of Physical Therapy, Faculty of Allied Health Sciences, Chulalongkorn University, Bangkok, Thailand
-
Received:2023-07-04Accepted:2023-01-18Published:2024-03-31Online:2024-03-05 -
Contact:* E-mail:premtip.t@chula.ac.th .
Cite this article
Ruchada Sriamad, Sirinut Chaiduang, Thaniya Klinsophon, Premtip Thaveeratitham. Body Positions Alter Hemodynamics and Respiration in Healthy Adults: A Systematic Review and Meta-Analysis[J].Chinese Medical Sciences Journal, 2024, 39(1): 29-45.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
Table 1.
Summary of evidence for the effects of body positions on hemodynamics and respiration"
| Outcomes | Comparators (positions) | Mean differences (95% CI) | No. participants | No. studies | Quality of evidence (GRADE) |
|---|---|---|---|---|---|
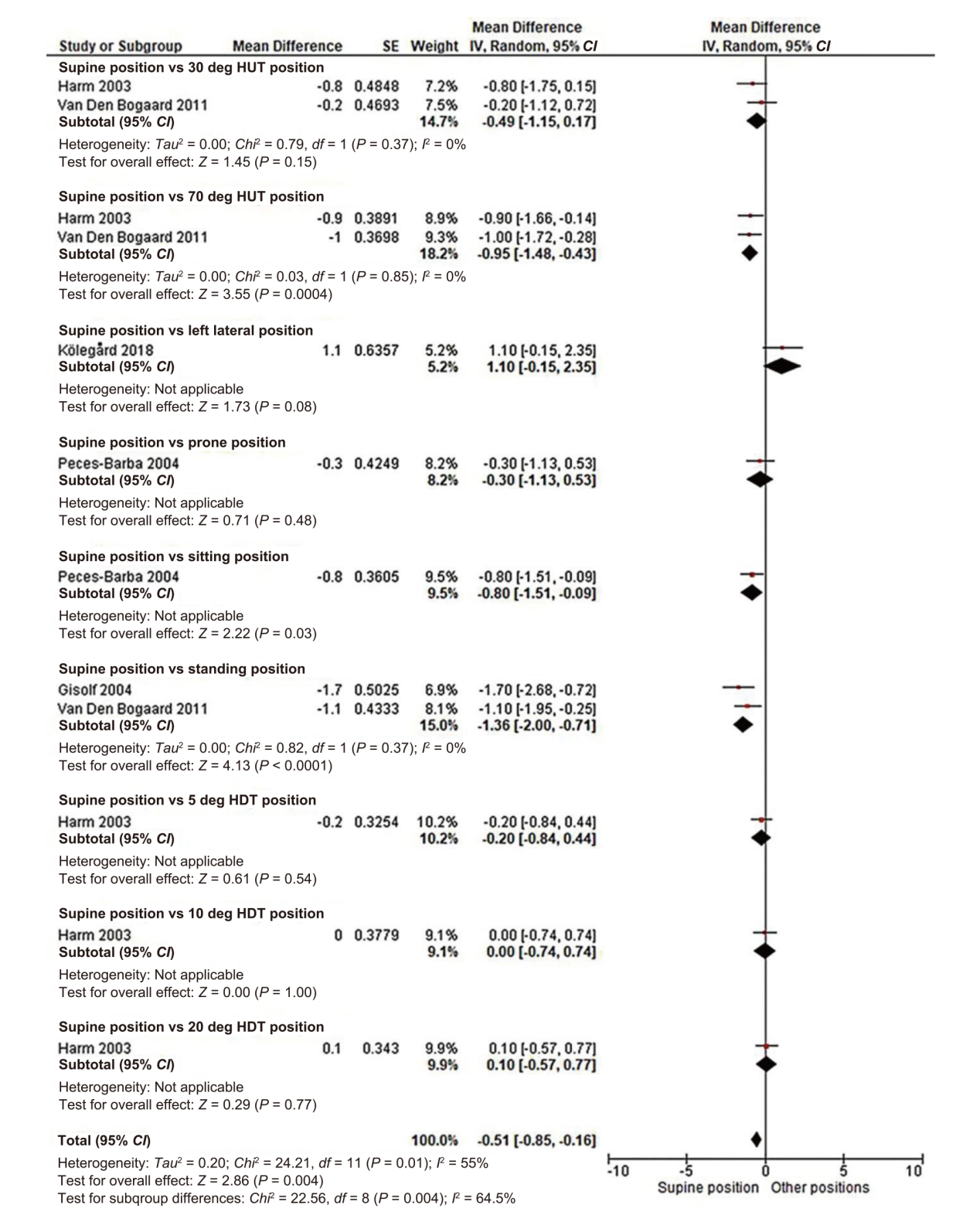
| CO | Supine versus 30 deg HUT | 0.49 (-0.17, 1.15) | 19 | 2 | Very low ? |
| Supine versus 70 deg HUT * | 0.95 (0.43, 1.48) | 19 | 2 | Low §, ?,|| | |
| Supine versus left lateral | -1.10 (-2.35, 0.15) | 12 | 1 | Low §, ?,|| | |
| Supine versus prone | 0.30 (-0.53, 1.13) | 10 | 1 | Low §, ?,|| | |
| Supine versus sitting * | 0.86 (0.33, 1.38) | 23 | 3 | Low §, ?, ?, || | |
| Supine versus standing * | 1.78 (0.41, 3.15) | 18 | 2 | Moderate §, ?,|||| | |
| Supine versus 5 deg HDT | 0.20 (-0.44, 0.84) | 9 | 1 | Very low §, ? | |
| Supine versus 10 deg HDT | 0.00 (-0.74, 0.74) | 9 | 1 | Very low §, ? | |
| Supine versus 20 deg HDT | -0.10 (-0.77, 0.57) | 9 | 1 | Very low §, ? | |
| 30 deg Fowler’s versus 60 deg Fowler’s | -0.10 (-0.51, 0.31) | 10 | 1 | Very low §, ? | |
| 60 deg HUT versus 60 deg HUT with left lateral (saddle-supported tilt) | -0.90 (-2.07, 0.27) | 12 | 1 | Low §, ?, || | |
| 60 deg HUT versus 60 deg HUT with left lateral (footboard-supported tilt) | -0.90 (-1.87, 0.07) | 12 | 1 | Low §, ?, || | |
| SBP | Supine versus 30 deg HUT | 1.30 (-8.44, 11.04) | 10 | 1 | Moderate §, ?, |||| |
| Supine versus 70 deg HUT | 3.30 (-4.84, 11.44) | 10 | 1 | Moderate §, ?, |||| | |
| Supine versus left lateral | 4.00 (-5.28, 13.28) | 12 | 1 | Moderate §, ?, |||| | |
| Supine versus standing | 1.30 (-7.64, 10.24) | 10 | 1 | Moderate §, ?, |||| | |
| 30 deg Fowler’s versus 60 deg Fowler’s | -2.80 (-13.34, 7.74) | 10 | 1 | Moderate §, |||| | |
| 60 deg HUT versus 60 deg HUT with left lateral (saddle-supported tilt) | -5.00 (-14.21, 4.21) | 12 | 1 | Moderate §, ??, |||| | |
| 60 deg HUT versus 60 deg HUT with left lateral (footboard-supported tilt) | 0.00 (-8.84, 8.84) | 12 | 1 | Very low §, ? | |
| DBP | Supine versus 30 deg HUT | -8.00 (-20.53, 4.53) | 10 | 1 | Moderate §, ?, |||| |
| Supine versus 70 deg HUT | -10.30 (-22.80, 2.20) | 10 | 1 | Moderate §, ?, |||| | |
| Supine versus left lateral | 2.00 (-4.91, 8.91) | 12 | 1 | Moderate §, ?, |||| | |
| Supine versus standing | -?.70 (-22.12, 2.72) | 10 | 1 | Moderate §, ?, |||| | |
| 30 deg Fowler’s versus 60 deg Fowler’s | -3.30 (-11.57, 4.97) | 10 | 1 | Moderate §, ??, |||| | |
| 60 deg HUT versus 60 deg HUT with left lateral (saddle-supported tilt) | -2.00 (-8.12, 4.12) | 12 | 1 | Moderate §, ??, |||| | |
| 60 deg HUT versus 60 deg HUT with left lateral (footboard-supported tilt) | 1.00 (-3.80, 5.80) | 12 | 1 | Low §, ?, || | |
| SVR | Supine versus 30 deg HUT | -175.33 (-354.77, 4.11) | 19 | 2 | Moderate §, ?, ?, |||| |
| Supine versus 70 deg HUT * | -380.84 (-623.86, -137.82) | 19 | 2 | Moderate §, ?, ?, |||| | |
| Supine versus 20 deg HDT | -31.00 (-159.06, 97.06) | 9 | 1 | Moderate §, ?, ?, |||| | |
| Supine versus standing * | -481.00 (-546.24, -415.76) | 10 | 1 | Moderate §, ?, ?, |||| | |
| 30 deg Fowler’s versus 60 deg Fowler’s | -30.90 (-143.92, 82.12) | 10 | 1 | Very low §, ?, ? | |
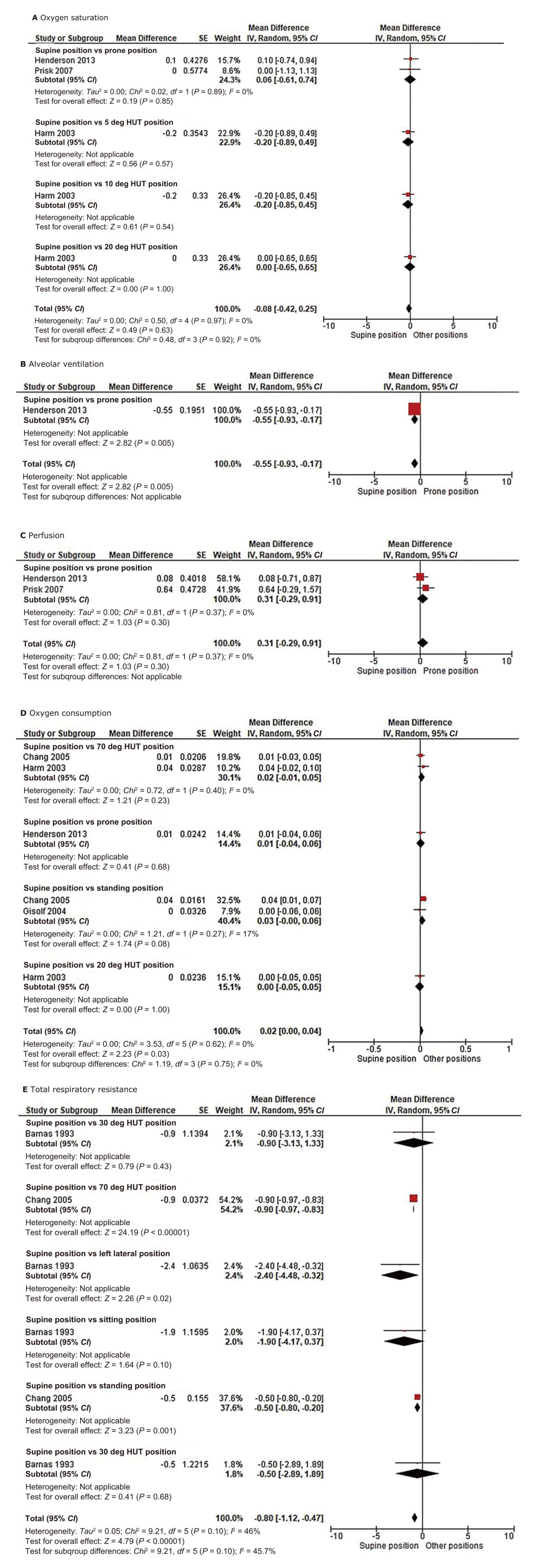
| SpO2 | Supine versus prone | -0.10 (-0.94, 0.74) | 13 | 2 | Very low §, ? |
| Supine versus 5 deg HDT | 0.20 (-0.49, 0.89) | 9 | 1 | Very low §, ? | |
| Supine versus 10 deg HDT | 0.20 (-0.45, 0.85) | 9 | 1 | Very low §, ? | |
| Supine versus 20 deg HDT | 0.00 (-0.65, 0.65) | 9 | 1 | Very low §, ? | |
| VA | Supine versus prone * | 0.55 (0.17, 0.93) | 7 | 1 | Very low §, ? |
| Q | Supine versus prone | -0.32 (-0.92, 0.28) | 13 | 2 | Very low ? |
| VO2 | Supine versus 70 deg HUT | -0.02 (-0.05, 0.01) | 29 | 2 | Very low ? |
| Supine versus prone | -0.01 (-0.06, 0.04) | 7 | 1 | Very low §, ? | |
| Supine versus standing | -0.03 (-0.06, -0.00) | 28 | 2 | Very low ? | |
| Supine versus 20 deg HDT | 0.00 (-0.05, 0.05) | 9 | 1 | Very low §, ? | |
| Rrs | Supine versus 30 deg HUT | 0.90 (-1.33, 3.13) | 7 | 1 | Low §, ?,|| |
| Supine versus 70 deg HUT * | 0.90 (0.83, 0.97) | 20 | 1 | Low §, ?,|| | |
| Supine versus left lateral * | 2.40 (0.32, 4.48) | 7 | 1 | Moderate §, ?,|||| | |
| Supine versus sitting | 1.90 (-0.37, 4.17) | 7 | 1 | Moderate §, ?, |||| | |
| Supine versus 30 deg HDT | 0.50 (-1.89, 2.89) | 7 | 1 | Very low §, ? | |
| Supine versus standing * | 0.50 (0.20, 0.80) | 20 | 1 | Very low §, ? | |
| Sitting versus 30 deg HUT | -1.00 (-3.23, 1.23) | 7 | 1 | Low §, ?, || | |
| Sitting versus left lateral | 0.50 (-1.58, 2.58) | 7 | 1 | Very low §, ? | |
| Sitting versus 30 deg HDT | -1.40 (-3.79, 0.99) | 7 | 1 | Moderate §, ?, |||| | |
| 30 deg HUT versus left lateral | 1.50 (-0.86, 3.86) | 7 | 1 | Moderate §, ?, |||| | |
| 30 deg HUT versus 30 deg HDT | -0.40 (-3.04, 2.24) | 7 | 1 | Very low §, ? | |
| Left lateral versus 30 deg HDT | -1.90 (-4.41, 0.61) | 7 | 1 | Moderate §, ?, |||| |
| 1. | Breathe S. Your lungs and exercise. NIH 2016;12(1):97-100. doi: 10.1183/20734735. |
| 2. | Hart EC, Charkoudian N, Wallin BG, et al. Sex differences in sympathetic neural-hemodynamic balance: implications for human blood pressure regulation. Hypertension 2009;53(3):571-76. doi: 10.1161/HYPERTENSIONAHA.108.126391. |
| 3. | LoMauro A, Aliverti A. Sex differences in respiratory function. Breathe 2018; 14(2):131-40. doi: 10.1183/20734735.000318. |
| 4. | Wolsk E, Bakkestrøm R, Thomsen JH, et al. The influence of age on hemodynamic parameters during rest and exercise in healthy individuals. JACC: Heart Failure 2017;5(5):337-46. doi: 10.1016/j.jchf.2016.10.012. |
| 5. | Fujimoto N, Borlaug BA, Lewis GD, et al. Hemodynamic responses to rapid saline loading: the impact of age, sex, and heart failure. Circ 2013;127(1):55-62. doi: 10.1161/CIRCULATIONAHA.112.111302. |
| 6. | Stelfox HT, Ahmed SB, Ribeiro RA, et al. Hemodynamic monitoring in obese patients: the impact of body mass index on cardiac output and stroke volume. Crit Care Med 2006;34(4):1243-46. doi: 10.1097/01.CCM.0000208358.27005.F4. |
| 7. | Cheng Y, Macera C, Addy C, et al. Effects of physical activity on exercise tests and respiratory function. BJSM 2003;37(6):521-28. doi: 10.1136/bjsm.37.6.521. |
| 8. | Bhatti U, Laghari ZA, Syed BM. Effect of body mass index on respiratory parameters: A cross-sectional analytical Study. Pak J Med Sci 2019;35(6):1724-29. doi: 10.12669/pjms.35.6.746. |
| 9. | Frerichs I, Braun P, Dudykevych T, et al. Distribution of ventilation in young and elderly adults determined by electrical impedance tomography. RESPNB 2004;143(1):63-75. doi: 10.1016/j.resp.2004.07.014. |
| 10. | Johnson KL, Meyenburg T. Physiological rationale and current evidence for therapeutic positioning of critically ill patients. AACN Adv Crit Care 2009;20(3):228-40. |
| 11. | Gisolf J, Wilders R, Immink RV, et al. Tidal volume, cardiac output and functional residual capacity determine end-tidal CO2 transient during standing up in humans. J Physiol 2004;554(2):579-90. doi: 10.1113/jphysiol.2003.056895. |
| 12. | Harms MP, van Lieshout JJ, Jenstrup M, et al. Postural effects on cardiac output and mixed venous oxygen saturation in humans. Exp Physiol 2003;88(5):611-16. doi: 10.1113/eph8802580. |
| 13. | Kawakami Y, Shida A, Murao M. The effects of posture on capillary blood flow pulse and gas exchange in the lungs of man. Jpn circ j 1980;44(5):327-33. doi: 10.1253/jcj.44.327. |
| 14. | Lundin G, Thomson D. Cardiac output in the supine and sitting position determined by a CO2 method. Acta Physiologica Scandinavica 1966;66(1-2):129-32. |
| 15. | Norsk P. Gravitational stress and volume regulation. Clin Physiol 1992;12(5):505-26. doi:10.1111/j.1475-097x.1992.tb00355.x. |
| 16. | Norsk P, Stadeager C, Johansen LB, et al. Volume-homeostatic mechanisms in humans during a 12-h posture change. J Appl Physiol 1993;75(1):349-56. doi: 10.1152/jappl.1993.75.1.349. |
| 17. | Van den Bogaard B, Westerhof BE, Best H, et al. Arterial wave reflection decreases gradually from supine to upright. Blood pressure 2011;20(6):370-75. doi: 10.3109/08037051.2011.588484 |
| 18. | Klijn E, Niehof S, Johan Groeneveld A, et al. Postural change in volunteers: sympathetic tone determines microvascular response to cardiac preload and output increases. Clin Auton Res 2015;25(6):347-54. doi: 10.1007/s10286-015-0286-x. |
| 19. | Watanabe N, Reece J, Polus BI. Effects of body position on autonomic regulation of cardiovascular function in young, healthy adults. Chiropr Osteopat 2007;15(1):1-8. doi: 10.1186/1746-1340-15-19 |
| 20. | Levick JR. Chapter 1 - Overview of the cardiovascular system. In: Levick JR, editor. An Introduction to Cardiovascular Physiology: Butterworth-Heinemann; 1991. p. 1-12. doi: 10.1016/B978-0-7506-1028-5.50004-4. |
| 21. | Henderson AC, Sá RC, Theilmann RJ, et al. The gravitational distribution of ventilation-perfusion ratio is more uniform in prone than supine posture in the normal human lung. J Appl Physiol 2013;115(3):313-24. doi: 10.1152/japplphysiol.01531.2012. |
| 22. | Nyren S, Mure M, Jacobsson H, et al. Pulmonary perfusion is more uniform in the prone than in the supine position: scintigraphy in healthy humans. J Appl Physiol 1999;86(4):1135-41. doi: 10.1152/jappl.1999.86.4.1135. |
| 23. | Chang AT, Boots RJ, Brown MG, et al. Ventilatory changes following head-up tilt and standing in healthy subjects. Eur J Appl Physiol 2005;95(5):409-17. doi: 10.1007/s00421-005-0019-2. |
| 24. | Lindahl SG. Using the prone position could help to combat the development of fast hypoxia in some patients with COVID-19. Acta Paediatr 2020;109(8):1539-44. doi: 10.1111/apa.15382. |
| 25. | Liu L, Xie J, Wang C, et al. Prone position improves lung ventilation-perfusion matching in non-intubated COVID-19 patients: a prospective physiologic study. Crit Care 2022;26(1):193. doi: 10.1186/s13054-022-04069-y. |
| 26. | Nyren S, Radell P, Lindahl SG, et al. Lung ventilation and perfusion in prone and supine postures with reference to anesthetized and mechanically ventilated healthy volunteers. ASA 2010;112(3):682-7. doi: 10.1097/ALN.0b013e3181cf40c8. |
| 27. | Barnas GM, Green MD, Mackenzie CF, et al. Effect of posture on lung and regional chest wall mechanics. ASA 1993;78(2):251-9. doi: 10.1097/00000542-199302000-00007. |
| 28. | Page MJ, McKenzie JE, Bossuyt PM, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. Bmj 2021; 372:n71. doi: 10.1136/bmj.n71. |
| 29. | Shamseer L, Moher D, Clarke M, et al. Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015: elaboration and explanation. BMJ 2015; 349:g7647. doi: 10.1136/bmj.g7647. |
| 30. | Downs SH, Black N. The feasibility of creating a checklist for the assessment of the methodological quality both of randomised and non-randomised studies of health care interventions. JECH 1998;52(6):377-84. doi: 10.1136/jech.52.6.377. |
| 31. | Higgins J. Cochrane handbook for systematic reviews of interventions. Version 5.1.0. [updated March 2011]. The Cochrane Collaboration. www cochrane-handbook org. 2011. |
| 32. | Guyatt G, Oxman AD, Akl EA, et al. GRADE guidelines: 1. Introduction-GRADE evidence profiles and summary of findings tables. J. Clin. Epidemiol 2011;64(4):383-94. doi: 10.1016/j.jclinepi.2010.04.026. |
| 33. |
Santesso N, Carrasco-Labra A, Langendam M, et al. Improving GRADE evidence tables part 3: detailed guidance for explanatory footnotes supports creating and understanding GRADE certainty in the evidence judgments. J Clin Epidemiol 2016; 74:28-39. doi: 10.1016/j.jclinepi.2015.12.006
pmid: 26796947 |
| 34. | Schünemann HJ, Oxman AD, Brozek J, et al. Grading quality of evidence and strength of recommendations for diagnostic tests and strategies. Bmj 2008;336(7653):1106-10. doi: 10.1136/bmj.39500.677199.AE. |
| 35. | Cohen J. Statistical power analysis for the behavioral sciences. 2nd ed. L. Erlbaum Associates Hillsdale, N.J.; 1988. |
| 36. | Maher JM, Markey JC, Ebert-May D. The other half of the story: effect size analysis in quantitative research. CBE Life Sci Educ 2013;12(3):345-51. doi:10.1187/cbe.13-04-0082. |
| 37. | Kölegård R, Da Silva C, Siebenmann C, et al. Cardiac performance is influenced by rotational changes of position in the transversal plane, both in the horizontal and in the 60° head-up postures. Clin. Physiol Funct Imaging 2018;38(6):1021-8. doi: 10.1111/cpf.12520. |
| 38. | Kubota S, Endo Y, Kubota M, et al. Effects of trunk posture in Fowler’s position on hemodynamics. Auton Neurosci 2015; 189:56-9. doi: 10.1016/j.autneu.2015.01.002. |
| 39. | Peces-Barba G, Rodríguez-Nieto MJ, Verbanck S, et al. Lower pulmonary diffusing capacity in the prone vs. supine posture. J. Appl. Physiol 2004;96(5):1937-42. doi: 10.1152/japplphysiol.00255.2003. |
| 40. | Prisk GK, Yamada K, Henderson AC, et al. Pulmonary perfusion in the prone and supine postures in the normal human lung. J Appl Physiol 2007;103(3):883-94. doi: 10.1152/japplphysiol.00292.2007. |
| 41. | Zhang H, Li JK. Noninvasive monitoring of transient cardiac changes with impedance cardiography. Cardiovasc Eng 2008;8(4):225-31. doi: 10.1007/s10558-008-9062-z. |
| 42. | Patel HN, Miyoshi T, Addetia K, et al. Normal values of cardiac output and stroke volume according to measurement technique, age, sex, and ethnicity: results of the world alliance of societies of echocardiography study. JASE 2021;34(10):1077-85. doi: 10.1016/j.echo.2021.05.012. |
| 43. | Kaku K, Takeuchi M, Otani K, et al. Age-and gender-dependency of left ventricular geometry assessed with real-time three-dimensional transthoracic echocardiography. JASE 2011;24(5):541-7. doi: 10.1016/j.echo.2011.01.011. |
| 44. | Hedenstierna G. Effects of body position on ventilation/perfusion matching. APICE. Springer; 2005:3-15. doi: 10.1007/88-470-0351-2_1. |
| 45. | Van Empel VP, Kaye DM, Borlaug BA. Effects of healthy aging on the cardiopulmonary hemodynamic response to exercise. Am J Card 2014;114(1):131-5. doi: 10.1016/j.amjcard.2014.04.011. |
| 46. | Chahal NS, Lim TK, Jain P, et al. Population-based reference values for 3D echocardiographic LV volumes and ejection fraction. JACC 2012;5(12):1191-7. doi: 10.1016/j.jcmg.2012.07.014. |
| 47. | De Simone G, Pasanisi F. Systolic, diastolic and pulse pressure: pathophysiology. Heart J Suppl 2001;2(4):359-62. |
| 48. | Ceylan B, Khorshid L, Güneş ÜY, et al. Evaluation of oxygen saturation values in different body positions in healthy individuals. J Clin Nurs 2016;25(7-8):1095-100. doi: 10.1111/jocn.13189. |
| 49. | Rohdin M, Petersson J, Sundblad P, et al. Effects of gravity on lung diffusing capacity and cardiac output in prone and supine humans. J Appl Physiol 2003;95(1):3-10. doi: 10.1152/japplphysiol.01154.2002. |
| 50. | Hopkins E, Sharma S. Physiology, functional residual capacity. 2022. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishaing; 2023. |
| 51. | Selvi EC, K KVR, Malathi. Should the Functional Residual Capacity be Ignored?. J Clin Diagn Res 2013;7(1):43-5. doi: 10.7860/JCDR/2012/4876.2666. |
| [1] | Wen-jing Li, Yi-ping Hu*, Min-min Zhu. Assessment of Stroke Volume Variation Perioperatively by Using Arterial Pressure with Cardiac Output [J]. Chinese Medical Sciences Journal, 2015, 30(2): 95-99. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||
|