Chinese Medical Sciences Journal ›› 2020, Vol. 35 ›› Issue (4): 289-296.doi: 10.24920/003759
• Original Article • Next Articles
Ultrasound-Guided Transmuscular Quadratus Lumbar Block Reduces Opioid Consumption after Laparoscopic Partial Nephrectomy
Xulei Cui1, Xu Li1, Minna Li1, Yuelun Zhang2, Yi Xie3, Weigang Yan3, Yushi Zhang3, Zhigang Ji3, Yuguang Huang1, *( )
)
- 1Anesthesiology Department, Peking Union Medical College Hospital,Chinese Academy of Medical Sciences & Peking Union Medical College, Beijing 100730, China
2Central Research Laboratory, Peking Union Medical College Hospital,Chinese Academy of Medical Sciences & Peking Union Medical College, Beijing 100730, China
3Urology Department, Peking Union Medical College Hospital,Chinese Academy of Medical Sciences & Peking Union Medical College, Beijing 100730, China
-
Received:2020-04-20Accepted:2020-06-29Published:2020-12-31Online:2020-10-18 -
Contact:Yuguang Huang E-mail:garybeijing@163.com
| This RCT study provide favorable evidence of evaluating the clinical value of ultrasound-guided transmuscular quadratus lumbar block in reducing opioid consumption in patients undertaking retroperitoneal procedures. |
Cite this article
Xulei Cui, Xu Li, Minna Li, Yuelun Zhang, Yi Xie, Weigang Yan, Yushi Zhang, Zhigang Ji, Yuguang Huang. Ultrasound-Guided Transmuscular Quadratus Lumbar Block Reduces Opioid Consumption after Laparoscopic Partial Nephrectomy[J].Chinese Medical Sciences Journal, 2020, 35(4): 289-296.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
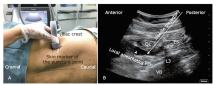
Figure 1.
The ultrasound-guided TQLB technique in this study. (A) Ultrasound probe position of scanning at the posterior axillary line immediately above the iliac crest and the puncture point for TQLB. (B) An ultrasonic image corresponding to the ultrasound scanning in (A) showing needle trajectory and spread of local anesthetics after injection. ES, erector spinae; PM, psoas major; QL, quadratus lumborum; TP, transverse process; TQLB, transmuscular quadratus lumborum block; VB, vertebral body."
Table 1
Patient characteristics and intraoperative variables"
| Patient characteristics | Control (n = 30) | TQLB group (n = 30) | Statistics | P |
|---|---|---|---|---|
| Age [yrs, mean (SD)] | 55.5 (14.5) | 51.5 (9.0) | 1.284* | 0.204 |
| Sex, male [n (%)] | 22 (73) | 19 (63) | 0.693? | 0.405 |
| Height [cm, mean (SD)] | 168.2 (8.2) | 168.3 (10.2) | -0.042* | 0.967 |
| Weight [kg, mean (SD)] | 71.7 (16.3) | 73.8(15.0) | -0.523* | 0.603 |
| ASA PS classification I/II (n) | 12/18 | 10/20 | 0.287? | 0.592 |
| Baseline HR [bpm, mean (SD)] | 74.7 (6.0) | 75.6 (7.2) | -0.547* | 0.587 |
| Baseline MBP [kPa mean (SD)] | 12.5 (1.1) | 12.7 (1.3) | -0.359* | 0.721 |
| Baseline NRS [median (IQR)] | 0 (0,0) | 0 (0,0) | 449.5# | 0.981 |
| intraoperative HR [bpm, mean (SD)] | 66.5 (7.7) | 65.9 (10.4) | 0.273* | 0.785 |
| intraoperative MBP [kPa, mean (SD)] | 11.9 (1.2) | 11.9 (0.0) | -0.059* | 0.953 |
| Duration of surgery [min, mean (SD)] | 109.5 (24.9) | 117.1 (32.9) | -1.013* | 0.315 |
| Hilar clamping time [min, median (IQR)] | 18.0 (7.0, 23.0) | 17.0 (2.5, 31.0) | 298.5# | 0.628 |
| Blood loss [mL, median (IQR)] | 200 (100, 300) | 225 (150, 502) | 347.0# | 0.100 |
| Urine output [mL, median (IQR)] | 200 (100, 300) | 225 (150, 503) | 362.5# | 0.188 |
| Crystalloid fluid [mL, mean (SD)] | 1,383.3 (387.8) | 1,441.4 (324.6) | -0.631* | 0.531 |
| expired isoflurane concentration [%, mean (SD)] | 1.3 (0.2) | 1.2 (0.2) | 0.385* | 0.702 |
| Intraoperative fentanyl [μg/kg, mean (SD)] | 2.4 (0.7) | 1.8 (0.8) | 3.088* | 0.003 |
| Intraoperative ephedrine [mg, median (IQR)] | 0 (0, 7.5) | 1.5 (0, 6.0) | 444.0# | 0.923 |
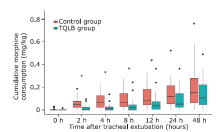
Figure 3.
Comparison of cumulative postoperative morphine consumption between TQLB gruop and the control group. Each box extends from the upper quartile to the lower quartile and is marked by a thick black line at the median. Whiskers reflect the upper and lower values after excluding outliers (>1.5 box lengths), which are represented by filled dots. TQLB, transmuscular quadratus lumborum block. * P<0.001; # P=0.01."
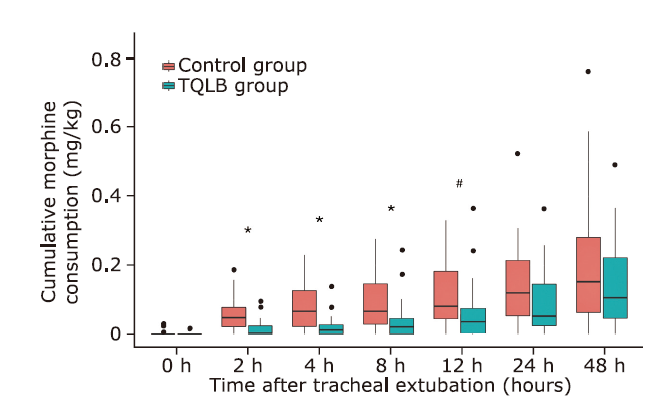
Table 2
Postoperative recovery-related data comparison between the TQLP patients and the controls"
| Postoperative recovery-related features | Control group (n = 30) | TQLB group (n = 30) | Statistics | P value |
|---|---|---|---|---|
| 24 h PONV (episode) [n (%)] | 14 (46.7) | 6 (20.0) | 4.800? | 0.028 |
| Time to first ambulation [h, mean (SD)] | 46.8 (18.6) | 53.3 (19.1) | -1.345* | 0.184 |
| Time to resumption of bowel movements [h, mean (SD)] | 35.6 (16.9) | 34.9 (17.5) | 0.164* | 0.870 |
| Patients’ satisfaction with anesthesia (very satisfied + satisfied) [n (%)] | 27 (90.0) | 29 (96.7) | 1.071? | 0.301 |
| QoR-15C score [mean (SD)] | ||||
| 72 h post-op | 123.9 (13.3) | 126.8 (12.4) | -0.815* | 0.419 |
| 120 h post-op | 131.9 (12.7) | 138.6 (10.3) | -2.164* | 0.035 |
| Post-op hospital stay [days, mean (SD)] | 6.3 (1.8) | 6.2 (1.7) | 0.149* | 0.882 |
| 1. |
Dam M, Moriggl B, Hansen CK, et al. The pathway of injectate spread with the transmuscular quadratus lumborum block: a cadaver study. Anesth Analg 2017; 125(1):303-12. doi: 10.1213/ANE.0000000000001922.
doi: 10.1213/ANE.0000000000001922 pmid: 28277325 |
| 2. | Blanco R. TAP block under ultrasound guidance: the description of a “no pops” technique. Reg Anesth Pain Med 2007; 32:S130. |
| 3. |
Murouchi T, Iwasaki S, Yamakage M. Quadratus lumborum block: analgesic effects and chronological ropivacaine concentrations after laparoscopic surgery. Reg Anesth Pain Med 2016; 41(2):146-50. doi: 10.1097/AAP.0000000000000349.
doi: 10.1097/AAP.0000000000000349 pmid: 26735154 |
| 4. |
Blanco R, Ansari T, Girgis E. Quadratus lumborum block for postoperative pain after caesarean section: a randomised controlled trial. Eur J Anaesthesiol 2015; 32(11):812-8. doi: 10.1097/EJA.0000000000000299.
doi: 10.1097/EJA.0000000000000299 pmid: 26225500 |
| 5. |
Blanco R, Ansari T, Riad W, et al. Quadratus lumborum block versus transversus abdominis plane block for postoperative pain after Cesarean delivery: a randomized controlled trial. Reg Anesth Pain Med 2016; 41(6):757-62. doi: 10.1097/AAP.0000000000000495.
doi: 10.1097/AAP.0000000000000495 pmid: 27755488 |
| 6. |
Børglum J, Moriggl B, Jensen K, et al. Ultrasound-guided transmuscular quadratus lumborum blockade. Br J Anaesth 2013; 111: eLetters supplement. doi: 1.1093/bja/el_9919.
doi: 10.1093/bja/aet392 pmid: 24233311 |
| 7. |
Hansen CK, Dam M, Bendtsen TF, et al. Ultrasound-guided quadratus lumborum blocks: definition of the clinical relevant endpoint of injection and the safest approach. A A Case Rep 2016; 6(2):39. doi: 10.1213/XAA.0000000000000270.
doi: 10.1213/XAA.0000000000000270 pmid: 26771297 |
| 8. | Corso RM, Piraccini E, Sorbello M, et al. Ultrasound-guided transmuscular quadratus lumborum block for perioperative analgesia in open nephrectomy. Minerva Anesthesiol 2017; 83(12):1334-5. doi: 10.23736/S0375-9393.17.12167-X. |
| 9. |
Warusawitharana C, Basar SHMA, Jackson BL, et al. Ultrasound guided continuous transmuscular quadratus lumborum analgesia for open renal surgery: a case series. J Clin Anesth 2017; 42(11):100-1. doi: 10.1016/j.jclinane.2017.08.025.
doi: 10.1016/j.jclinane.2017.08.025 |
| 10. |
Copik M, Bialka S, Daszkiewicz A, et al. Thoracic paravertebral block for postoperative pain management after renal surgery: a randomised controlled trial. Eur J Anaesthesiol 2017; 34(9):596-601. doi: 10.1097/EJA.0000000000000673.
doi: 10.1097/EJA.0000000000000673 pmid: 28731925 |
| 11. |
Bu XS, Zhang J, Zuo YX. Validation of the Chinese version of the quality of recovery-15 score and its comparison with the post-operative quality recovery scale patient. Patient 2016; 9(3):251-9. doi: 10.1007/s40271-015-0148-6.
pmid: 26518201 |
| 12. |
Nanidis TG, Antcliffe D, Kokkinos C, et al. Laparoscopic versus open live donor nephrectomy in renal transplantation: a meta-analysis. Ann Surg 2008; 247(1):58-70. doi: 10.1097/SLA.0b013e318153fd13.
doi: 10.1097/SLA.0b013e318153fd13 pmid: 18156924 |
| 13. | Vukovic N. Enhanced recovery after surgery protocols in major urologic surgery. Front Med (Lausanne) 2018; 5(4):93. doi: 10.3389/fmed.2018.00093. |
| 14. |
Karmakar MK. Thoracic paravertebral block. Anesthesiology 2001; 95(3):771-80. doi: 10.1097/00000542-200109000-00033
doi: 10.1097/00000542-200109000-00033 pmid: 11575553 |
| 15. |
Abdallah FW, Halpern SH, Aoyama K, et al. Will the real benefits of single-shot interscalene block please stand up? A systematic review and meta-analysis. Anesth Analg 2015; 120(5):1114-29. doi: 10.1213/ANE.0000000000000688.
doi: 10.1213/ANE.0000000000000688 pmid: 25822923 |
| 16. |
Lavand’homme P. Rebound pain after regional anesthesia in the ambulatory patient. Curr Opin Anaesthesiol 2018; 31(6):679-84. doi: 10.1097/ACO.0000000000000651.
pmid: 30124544 |
| 17. |
Kuthiala G, Chaudhary G. Ropivacaine: A review of its pharmacology and clinical use. Indian J Anaesth 2011; 55(2):104-10. doi: 10.4103/0019-5049.79875.
pmid: 21712863 |
| 18. |
Knight JB, Schott NJ, Kentor ML, et al. Neurotoxicity of common peripheral nerve block adjuvants. Curr Opin Anaesthesiol 2015; 28(5):598-604. doi: 10.1097/ACO.0000000000000222.
pmid: 26207854 |
| 19. |
Zhu Q, Li L, Yang Z, et al. Ultrasound guided continuous quadratus lumborum block hastened recovery in patients undergoing open liver resection: a randomized controlled, open-label trial. BMC Anesthesiol 2019; 19(1):23. doi: 10.1186/s12871-019-0692-z.
pmid: 30777027 |
| 20. |
Abdallah FW, Morgan PJ, Cil T, et al. Ultrasound-guided multilevel paravertebral blocks and total intravenous anesthesia improve the quality of recovery after ambulatory breast tumor resection. Anesthesiology 2014; 120(3):703-13. doi: 10.1097/ALN.0000436117.52143.bc.
doi: 10.1097/ALN.0000436117.52143.bc |
| 21. |
Carline L, McLeod GA, Lamb C. A cadaver study comparing spread of dye and nerve involvement after three different quadratus lumborum blocks. Br J Anaesth 2016; 117(3):387-94. doi: 10.1093/bja/aew224.
doi: 10.1093/bja/aew224 pmid: 27543534 |
| 22. |
Adhikary SD, El-Boghdadly K, Nasralah Z, et al. A radiologic and anatomic assessment of injectate spread following transmuscular quadratus lumborum block in cadavers. Anaesthesia 2017; 72(1):73-9. doi: 10.1111/anae.13647.
doi: 10.1111/anae.13647 pmid: 27730633 |
| 23. |
Abdulla MH, Johns EJ. The innervation of the kidney in renal injury and inflammation: a cause and consequence of deranged cardiovascular control. Acta Physiol 2017; 220(4):404-16. doi: 10.1111/apha.12856.
doi: 10.1111/apha.2017.220.issue-4 |
| 24. |
Elsharkawy H, El-Boghdadly K, Barrington M. Quadratus lumborum block: anatomical concepts, mechanisms, and techniques. Anesthesiology 2019; 130(2):322-35. doi: 10.1097/ALN.0000000000002524.
doi: 10.1097/ALN.0000000000002524 pmid: 30688787 |
| 25. |
Wikner M. Unexpected motor weakness following quadratus lumborum block for gynaecological laparoscopy. Anaesthesia 2017; 72(2):230-2. doi: 10.1111/anae.13754.
doi: 10.1111/anae.13754 pmid: 27891579 |
| 26. |
Carney J, Finnerty O, Rauf J, et al. Studies on the spread of local anaesthetic solution in transverses abdominis plane blocks. Anaesthesia 2011; 66(11):1023-30. doi: 10.1111/j.1365-2044.2011.06855.x.
doi: 10.1111/j.1365-2044.2011.06855.x |
| 27. |
Rozen WM, Tran TM, Ashton MW, et al. Refining the course of the thoracolumbar nerves: a new understanding of the innervation of the anterior abdominal wall. Clin Anat 2008; 21(4):325-33. doi: 10.1002/ca.20621.
pmid: 18428988 |
| 28. | Bendtsen TF, Kølsen JAP. Regional analgesia. In: Rasmussen LS, Steinmetz J (Eds). Anæstesi, 4th ed. København: FADL’s Forlag; 2014. 143e72. |
| 29. |
Griffiths JD, Barron FA, Grant S, et al. Plasma ropivacaine concentrations after ultrasound-guided transversus abdominis plane block. Br J Anaesth 2010; 105(6):853-6. doi: 10.1093/bja/aeq255.
doi: 10.1093/bja/aeq255 pmid: 20861094 |
| [1] | Chen Xing,Wang Jianfeng,Ding Zhenshan,Zhou Xiaofeng. Solitary Fibrous Tumor of the Kidney Treated with Laparoscopic Partial Nephrectomy: A Case Report [J]. Chinese Medical Sciences Journal, 2018, 33(1): 64-68. |
| [2] | Ge Qu, Xu-lei Cui, Hong-ju Liu, Zhi-gang Ji, Yu-guang Huang. Ultrasound-guided Transversus Abdominis Plane Block Improves Postoperative Analgesia and Early Recovery in Patients Undergoing Retroperitoneoscopic Urologic Surgeries: A Randomized Controlled Double-blinded Trial [J]. Chinese Medical Sciences Journal, 2016, 31(3): 137-141. |
| [3] | Jing Fu, Shan Ye, Hua-jian Ye. Retroperitoneal Versus Transperitoneal Laparoscopic Partial Nephrectomy: A Systematic Review and Meta-analysis [J]. Chinese Medical Sciences Journal, 2015, 30(4): 239-244. |
| [4] | Ji-rui Niu, Quan-zong Mao, and Zhi-gang Ji. Open Partial Nephrectomy in Solitary Kidney with Multiple Renal Cell Carcinoma: a Case Report [J]. Chinese Medical Sciences Journal, 2011, 26(4): 249-250. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||
|