Chinese Medical Sciences Journal ›› 2023, Vol. 38 ›› Issue (4): 257-264.doi: 10.24920/004202
• Original Article • Next Articles
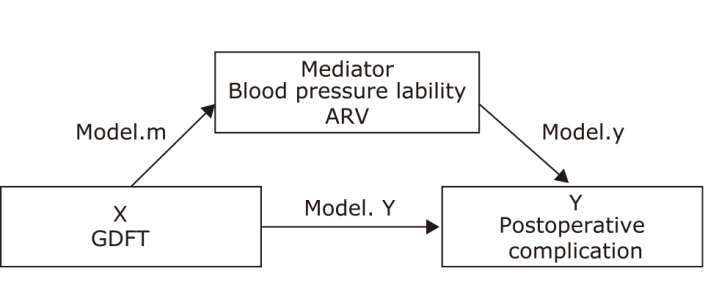
Intraoperative Blood Pressure Lability Acts as a Key Mediator in the Impacts of Goal-Directed Fluid Therapy on Postoperative Complications in Patients Undergoing Major Spine Surgery
Lu Che, Jia-Wen Yu, Yue-Lun Zhang, Li Xu( ), Yu-Guang Huang
), Yu-Guang Huang
- Department of Anesthesiology, Peking Union Medical College Hospital, Chinese Academy of Medical Sciences & Peking Union Medical College, Beijing 100730, China
-
Received:2022-12-22Accepted:2023-07-12Published:2023-12-30Online:2023-09-06 -
Contact:Li Xu E-mail:pumchxuli@163.com
Cite this article
Lu Che,Jia-Wen Yu,Yue-Lun Zhang,Li Xu,Yu-Guang Huang. Intraoperative Blood Pressure Lability Acts as a Key Mediator in the Impacts of Goal-Directed Fluid Therapy on Postoperative Complications in Patients Undergoing Major Spine Surgery[J].Chinese Medical Sciences Journal, 2023, 38(4): 257-264.
share this article
Add to citation manager EndNote|Reference Manager|ProCite|BibTeX|RefWorks
Table 1.
Baseline characteristics of the GDFT group and the control group"
| Variables | GDFT group (n = 150) | Control group (n = 150) | P value |
|---|---|---|---|
| Age (yrs, mean ± SD) | 57.8 ± 17.2 | 59.2 ± 13.8 | 0.448 |
| Sex, male [n (%)] | 61 (40.7) | 63 (42.0) | 0.725 |
| BMI (kg/m2, mean ± SD ) | 25.4 ± 3.8 | 25.4 ± 3.3 | |
| ASA score [n (%)] | 0.971 | ||
| ≤ Ⅱ | 141 (94.0) | 144 (91.0) | |
| > Ⅱ | 9 (6.0) | 6 (9.0) | |
| Comorbidity [n (%)] | |||
| Hypertension | 66 (44.0) | 61 (40.7) | 0.514 |
| Coronary artery disease | 10 (6.7) | 10 (6.7) | 0.987 |
| Diabetes mellitus type Ⅱ | 21 (14.0) | 25 (16.8) | 0.521 |
| Baseline Hb (g·L-1, mean ± SD) | 136.0 ± 13.2 | 134.7 ± 19.4 | 0.486 |
| Baseline HR (bpm, mean ± SD) | 77.0 ± 9.2 | 79.0 ± 10.5 | 0.162 |
| Baseline SBP (mmHg, mean ± SD) | 129.5 ± 15.9 | 132.3 ± 15.3 | 0.121 |
| Baseline creatinine (μg·ml-1, mean ± SD) | 67.9 ± 19.3 | 67.1 ± 12.8 | 0.657 |
| Infused crystalloids [ml·kg-1·h-1, median (IQR)] | 7.2 (4.6-9.8) | 7.4 (5.1-9.7) | 0.398 |
| Infused colloids [ml·kg-1·h-1, median (IQR)] | 1.6 (0.3-2.9) | 1.6 (0.3-2.9) | 0.893 |
| Vasopressor [n (%)] | 7 (4.67) | 20 (13.33) | 0.009 |
| Operation time [min, median (IQR)) | 184 (153-220) | 193 (156-225) | 0.404 |
| ARV (mmHg·min-1, median (IQR)) | 0.87 (0.53-1.25) | 1.73 (1.16-2.49) | <0.001 |
| TWA_MAP (mmHg, mean ± SD) | 82.7 ± 7.7 | 82.3 ± 9.5 | 0.219 |
Table 2.
Results of crude and adjusted analysis of the association with 30-day postoperative complications"
| Items | Crude | Adjusted* | |||||
|---|---|---|---|---|---|---|---|
| OR | 95% CI | P value | OR | 95% CI | P value | ||
| GDFT | 0.510 | 0.319, 0.815 | 0.005 | 0.460 | 0.278, 0.761 | 0.003 | |
| TWA_MAP | 0.922 | 0.892, 0.953 | <0.001 | 0.928 | 0.897, 0.960 | <0.001 | |
| ARV (mmHg·min-1) | 1.687 | 1.338, 2.126 | <0.001 | 1.634 | 1.278, 2.090 | <0.001 | |
| 1. | Messina A, Robba C, Calabrò L, et al. Association between perioperative fluid administration and postoperative outcomes: a 20-year systematic review and a meta-analysis of randomized goal-directed trials in major visceral/noncardiac surgery. Crit Care 2021; 25(1):43. doi: 10.1186/s13054-021-03464-1. |
| 2. |
Calvo-Vecino JM, Ripollés-Melchor J, Mythen MG, et al. Effect of goal-directed haemodynamic therapy on postoperative complications in low-moderate risk surgical patients: a multicentre randomised controlled trial (FEDORA trial). Br J Anaesth 2018; 120(4):734-44. doi: 10.1016/j.bja.2017.12.018.
pmid: 29576114 |
| 3. |
Che L, Zhang XH, Li X, et al. Outcome impact of individualized fluid management during spine surgery: a before-after prospective comparison study. BMC Anesthesiol 2020; 20(1):181. doi: 10.1186/s12871-020-01092-w.
pmid: 32698766 |
| 4. | Park S, Lee HC, Jung CW, et al. Intraoperative arterial pressure variability and postoperative acute kidney injury. Clin J Am Soc Nephrol 2020; 15(1):35-46. doi: 10.2215/cjn.06620619. |
| 5. | Wiórek A, Krzych Ł J. Intraoperative blood pressure variability predicts postoperative mortality in non-cardiac surgery—a Prospective Observational Cohort Study. Int J Environ Res Public Health 2019; 16(22):4380. doi: 10.3390/ijerph16224380. |
| 6. |
Li J, Zhao Y, Zhao M, et al. High variance of intraoperative blood pressure predicts early cerebral infarction after revascularization surgery in patients with Moyamoya disease. Neurosurg Rev 2020; 43(2):759-69. doi: 10.1007/s10143-019-01118-z.
pmid: 31203482 |
| 7. | Lizano-Díez I, Poteet S, Burniol-Garcia A, et al. The burden of perioperative hypertension/hypotension: a systematic review. PLoS One 2022; 17(2):e0263737. doi: 10.1371/journal.pone.0263737. |
| 8. |
Lee H, Cashin A, Lamb S, et al. A Guideline for Reporting Mediation Analyses of Randomized Trials and Observational Studies: The AGReMA Statement. JAMA 2021; 326(11):1045-56. doi: 10.1001/jama.2021.14075.
pmid: 34546296 |
| 9. |
Chen X, Zhu Y, Geng S, et al. Association of blood pressure variability and intima-media thickness with white matter hyperintensities in hypertensive patients. Front Aging Neurosci 2019; 11:192. doi: 10.3389/fnagi.2019.00192.
pmid: 31447663 |
| 10. |
Hansen TW, Thijs L, Li Y, et al. Prognostic value of reading-to-reading blood pressure variability over 24 hours in 8938 subjects from 11 populations. Hypertension 2010; 55(4):1049-57. doi: 10.1161/hypertensionaha.109.140798.
pmid: 20212270 |
| 11. |
Buis ML. Direct and indirect effects in a logit model. Stata J 2010; 10(1):11-29.
pmid: 22468140 |
| 12. |
Imai K, Keele L, Tingley D. A general approach to causal mediation analysis. Psychol Methods 2010; 15(4):309-34. doi: 10.1037/a0020761.
pmid: 20954780 |
| 13. | Valente MJ, Rijnhart JJM, Smyth HL, et al. Causal mediation programs in R, Mplus, SAS, SPSS, and Stata. Struct Equ Modeling 2020; 27(6):975-84. doi: 10.1080/10705511.2020.1777133. |
| 14. | Schoemann AM, Boulton AJ, Short SD. Determining power and sample size for simple and complex mediation models. Soc Psychol Personal Sci 2017; 8(4):379-86. doi: 10.1177/1948550617715068. |
| 15. | Luo MS. Perioperative goal-directed therapy in high-risk abdominal surgery. J Clin Anesth 2022; 78:110637. doi: 10.1016/j.jclinane.2021.110637. |
| 16. |
Zorrilla-Vaca A, Cata JP, Brown JK, et al. Goal-directed fluid therapy does not have an impact on renal outcomes in an enhanced recovery program. Ann Thorac Surg 2022; 114(6):2059-65. doi: 10.1016/j.athoracsur.2022.03.070.
pmid: 35452665 |
| 17. | Jessen MK, Vallentin MF, Holmberg MJ, et al. Goal-directed haemodynamic therapy during general anaesthesia for noncardiac surgery: a systematic review and meta-analysis. Br J Anaesth 2022; 128(3):416-33. doi: 10.1016/j.bja.2021.10.046. |
| 18. | Wei FF, Li Y, Zhang L, et al. Beat-to-beat, reading-to-reading, and day-to-day blood pressure variability in relation to organ damage in untreated Chinese. Hypertension 2014; 63(4):790-6. doi: 10.1161/hypertensionaha.113.02681. |
| 19. | Sachdeva R, Nightingale TE, Krassioukov AV. The blood pressure pendulum following spinal cord injury: implications for vascular cognitive impairment. Int J Mol Sci 2019; 20(10):2464. doi: 10.3390/ijms20102464. |
| 20. |
Leibowitz A, Grossman E, Berkovitch A, et al. The effect of head and neck radiotherapy on blood pressure and orthostatic hypotension in patients with head and neck tumors. Am J Hypertens 2018; 31(2):235-9. doi: 10.1093/ajh/hpx158.
pmid: 28985342 |
| 21. | Putowski Z, Czok M, Krzych Ł. The impact of intraoperative blood pressure variability on the risk of postoperative adverse outcomes in non-cardiac surgery: a systematic review. J Anes 2022; 36(2):316-22. doi: 10.1007/s00540-022-03035-w. |
| 22. | Südfeld S, Brechnitz S, Wagner J, et al. Post-induction hypotension and early intraoperative hypotension associated with general anaesthesia. Br J Anaes 2017; 119(1):57-64. doi: 10.1093/bja/aex127. |
| 23. | Zhao JB, Li YL, Xia DY, et al. Protective effect of targeted fluid therapy on patients with one-lung ventilation. Evid Based Complement Alternat Med 2022; 2022:7850031. doi: 10.1155/2022/7850031. |
| 24. | Chirnoaga D, Coeckelenbergh S, Ickx B, et al. Impact of conventional vs. goal-directed fluid therapy on urethral tissue perfusion in patients undergoing liver surgery: a pilot randomised controlled trial. Eur J Anaesthesiol 2022; 39(4):324-32. doi: 10.1097/eja.0000000000001615. |
| 25. | Wang DD, Li Y, Hu XW, et al. Comparison of restrictive fluid therapy with goal-directed fluid therapy for postoperative delirium in patients undergoing spine surgery: a randomized controlled trial. Perioper Med (Lond) 2021; 10(1):48. doi: 10.1186/s13741-021-00220-5. |
| 26. |
Khan AI, Fischer M, Pedoto AC, et al. The impact of fluid optimisation before induction of anaesthesia on hypotension after induction. Anaesthesia 2020; 75(5):634-41. doi: 10.1111/anae.14984.
pmid: 32030734 |
| 27. |
Fontanarosa P. Reporting findings from mediation analyses. JAMA 2021; 326(11):1057. doi: 10.1001/jama.2021.15786.
pmid: 34546315 |
| [1] | Lulu Ma, Xuerong Yu, Xisheng Weng, Jin Lin, Jin Jin, Wenwei Qian, Yuguang Huang. Possible Risk Factors for Severe Complications Occurring after Primary Total Knee Arthroplasty [J]. Chinese Medical Sciences Journal, 2022, 37(4): 303-308. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||
|